- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
Hip Dislocation Surgery Recovery and Advanced Stability Solutions
Understanding Hip Dislocation Surgery: Recovery and Advanced Solutions
Dealing with a joint instability can be a physically and emotionally taxing journey. hip dislocation surgery is often the definitive path for patients who suffer from chronic instability or acute traumatic injuries that cannot be managed through conservative physical therapy. Whether the goal is to restore mobility or prevent future dislocations, understanding the surgical process is the first step toward a successful recovery. In this guide, we explore the nuances of the procedure, the latest surgical techniques, and the critical role of post-operative support in regaining a full range of motion.
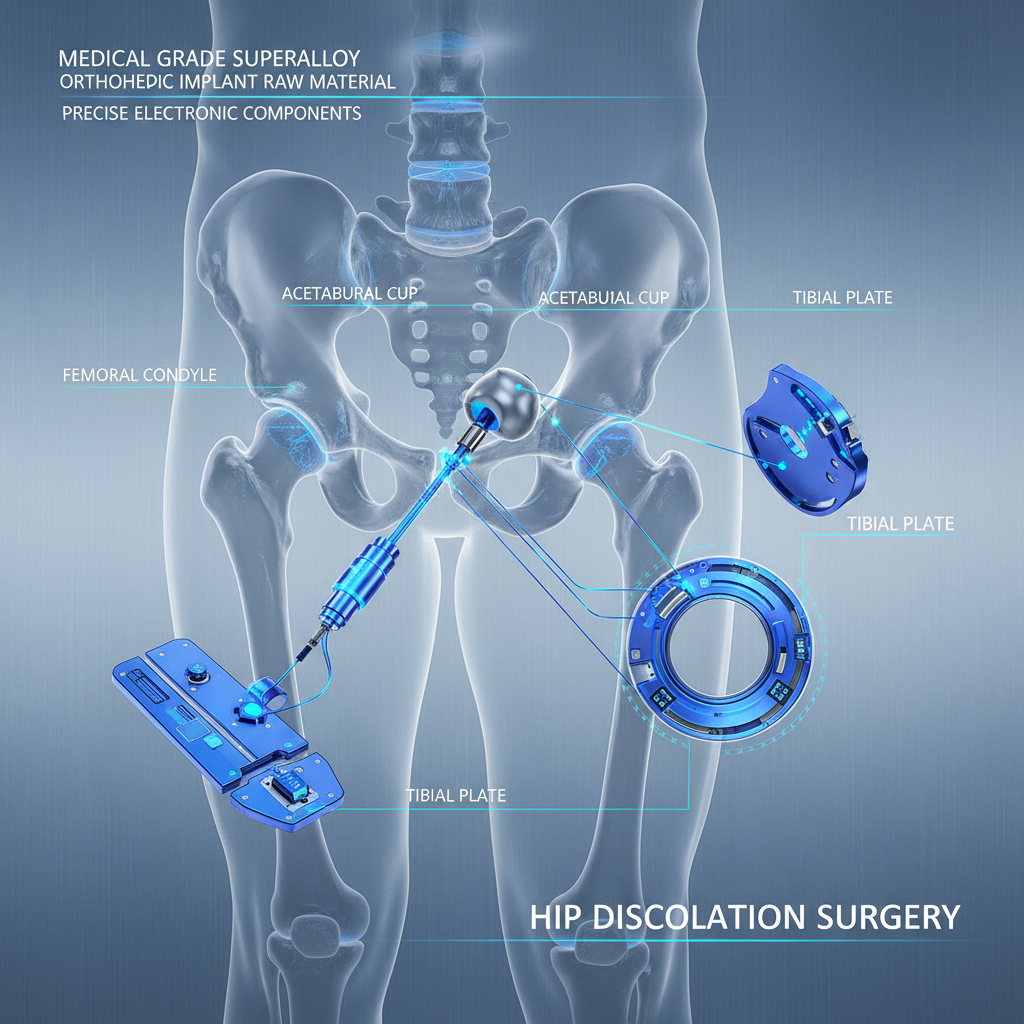
When is Hip Dislocation Surgery Necessary?
Not every hip injury requires an invasive procedure. However, chronic instability—where the hip pops out of the socket repeatedly—often necessitates surgical intervention to prevent permanent cartilage damage. Surgeons typically recommend hip dislocation surgery when there is a significant tear in the labrum or when the acetabulum (the socket) is too shallow to hold the femoral head securely. Early intervention is key to avoiding premature osteoarthritis and ensuring that the joint remains functional for years to come.
Clinical Indicators: Recurring dislocations, persistent pain despite physical therapy, structural abnormalities in the hip socket, and severe loss of joint stability.
Comparing Surgical Approaches for Hip Stability
Modern medicine offers several ways to address joint instability. Depending on the patient's age and the severity of the injury, a surgeon might choose between a minimally invasive arthroscopic approach or a more traditional open surgery. The choice often depends on whether the goal is simply to repair soft tissue or to physically reshape the bone to provide better coverage for the joint. Choosing the right method for hip dislocation surgery can significantly impact the speed of the initial recovery phase.
The Role of Immobilization in Hip Dislocation Surgery
Following a procedure, the stability of the joint is fragile. To ensure the surgical repairs set correctly, surgeons often employ stabilization tools. This is where high-quality casting and bracing come into play. Proper immobilization prevents accidental movement that could jeopardize the hip dislocation surgery outcomes. By limiting the range of motion in the early stages, patients can avoid re-injury while allowing the soft tissues and bones to heal in the correct alignment.

Recovery Milestones After Hip Dislocation Surgery
Recovery is a phased process. It begins with pain management and protecting the surgical site, eventually progressing to weight-bearing exercises. The key to long-term success is progressive loading. Rushing back into activity can lead to failure of the implants or sutures. For those recovering from hip dislocation surgery, the focus shifts from complete stillness to guided mobility, ensuring the joint is strengthened without being overstressed.
Recovery Phase Breakdown:
• Weeks 1-4: Protection, pain control, and limited weight-bearing.
• Weeks 5-12: Gradual increase in motion and physical therapy.
• Months 3-6: Strength building and return to daily activities.
• 6 Months+: Return to sports or high-impact activities (with approval).
Technical Specifications for Stabilization Support
For medical professionals and patients, selecting the right materials for post-surgical support is vital. Whether using a hip spica cast or a dynamic brace, the materials must be breathable yet rigid enough to prevent joint displacement. When supporting a patient after hip dislocation surgery, the following specifications are typically prioritized to ensure clinical effectiveness and patient comfort.
Long-term Outlook and Maintenance of Hip Health
The end of the clinical recovery period does not mean the end of care. To maintain the results of hip dislocation surgery, patients must adopt a lifestyle that supports joint longevity. This includes maintaining a healthy weight to reduce stress on the joint, continuing low-impact strengthening exercises, and attending regular follow-up appointments. By focusing on muscle balance—particularly strengthening the gluteus medius—patients can create a "natural brace" of muscle that protects the joint from future instability.
Conclusion: Reclaiming Mobility Through Precision Care
Recovering from a hip injury requires a combination of surgical precision, patient discipline, and high-quality support tools. Hip dislocation surgery offers a renewed lease on life for those struggling with chronic pain and instability. By adhering to strict post-operative protocols and utilizing professional stabilization equipment, patients can safely return to the activities they love. Remember, the journey to recovery is a marathon, not a sprint—patience and professional guidance are your best allies.
Frequently Asked Questions (FAQs)
How long is the recovery period after hip dislocation surgery?
The recovery timeline varies depending on the complexity of the procedure. For simple arthroscopic repairs, patients may return to light activities within a few weeks. However, for major reconstructions like a Periacetabular Osteotomy, full recovery can take six months to a year. The first 6-12 weeks are the most critical, as this is when the joint is most vulnerable and requires strict adherence to weight-bearing restrictions and immobilization protocols to ensure the surgery is successful.
Will I be able to return to sports after this surgery?
In most cases, yes. The primary goal of the surgery is to restore stability so that the patient can return to their normal lifestyle. However, the type of sport matters. Low-impact activities like swimming and cycling are usually encouraged early in the recovery process. High-impact or contact sports (like football or rugby) require a more extensive rehabilitation period and a final clearance from the surgeon to ensure the joint can handle the explosive forces involved without dislocating again.
What are the risks associated with hip dislocation surgery?
As with any major surgery, there are inherent risks, including infection, blood clots (DVT), and reactions to anesthesia. Specifically for hip surgery, there is a risk of nerve injury or the possibility that the joint may still experience instability if the underlying bone structure does not heal as expected. To minimize these risks, surgeons emphasize the use of high-quality post-operative supports and a strict physical therapy regimen. Regular check-ups and imaging (X-rays/MRI) are used to monitor the healing process closely.
How does stabilization support help in the healing process?
Stabilization supports, such as casts or specialized braces, act as an external skeleton. They hold the femoral head firmly within the acetabulum, preventing any micro-movements that could tear new sutures or disrupt bone grafting. This mechanical stability is crucial during the inflammatory and proliferative phases of healing. By ensuring the joint remains in the optimal anatomical position, these supports reduce the risk of surgical failure and allow the patient to move more confidently during the early stages of rehabilitation.
Get a Custom Solution!
Contact Us To Provide You With More Professional Services