- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
High riding humeral head treatment, simply put, is addressing a specific shoulder instability issue where the ball of the shoulder joint (the humeral head) sits too high within the socket (glenoid). This isn't just a sports injury thing, though it's common in athletes. It stems from cartilage damage, often after dislocations, and impacts quality of life – causing pain, clicking, and a feeling of instability. Addressing this early, and with the right approach, can mean the difference between returning to full function and chronic shoulder problems. We've seen a real uptick in these cases lately, driven by increased participation in overhead sports and a growing, more active aging population.
The global relevance lies in the increasing demand for effective orthopedic solutions. Aging populations worldwide are naturally seeing more degenerative joint issues. Furthermore, participation in sports and recreational activities continues to rise globally. According to the World Health Organization, musculoskeletal conditions are a leading cause of disability, impacting economies through lost productivity. Effective high riding humeral head treatment allows individuals to remain active, contributing to both personal wellbeing and economic output. The challenge is tailoring treatments – whether conservative or surgical – to the individual needs of patients and the resources available in different healthcare systems.
Essentially, high riding humeral head treatment aims to restore the normal biomechanics of the shoulder. It's not always about simply putting the ball back in the socket. Sometimes it requires procedures to deepen the socket, address labral tears, or even procedures to reshape the humeral head itself. It’s a delicate balance. It ties directly into the modern need for minimally invasive, patient-centered orthopedic care—getting people back to their lives with less pain and faster recovery times. This is a move away from the ‘one size fits all’ approach of the past, and towards personalized medicine.
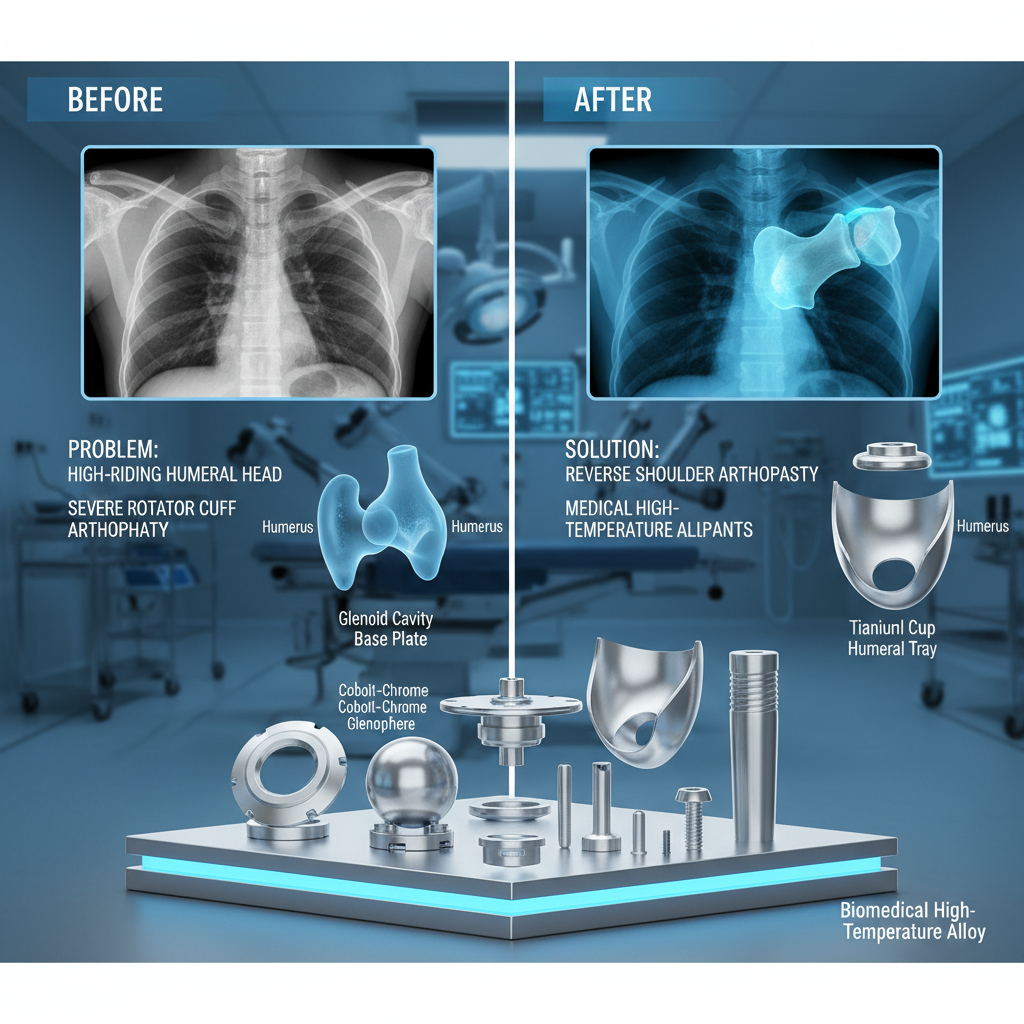
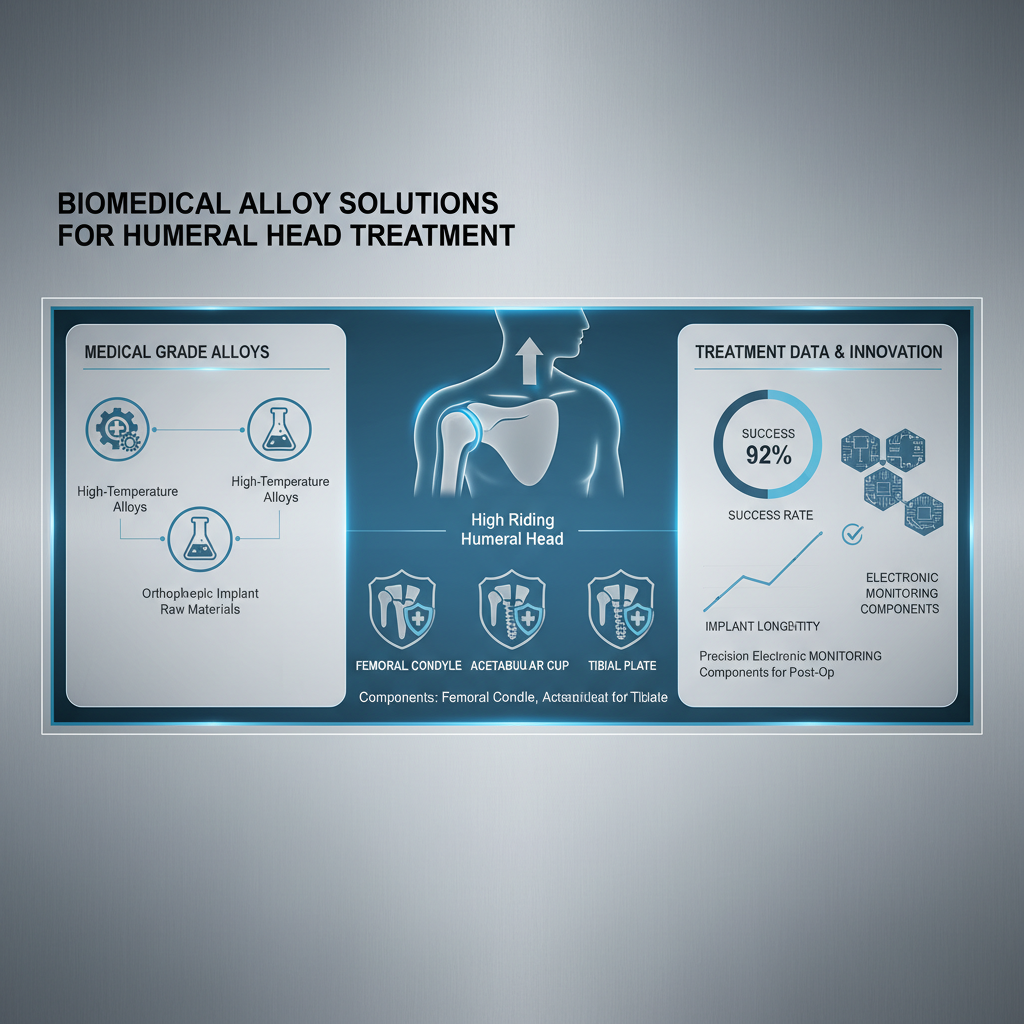
High riding humeral head treatment isn't just one thing. It's a spectrum of approaches, starting with conservative management like physical therapy to strengthen the surrounding muscles and improve stability. But frankly, that often only buys you time. The real challenge comes when conservative treatments fail, and you’re looking at surgical intervention. That’s where things get interesting. It’s about understanding why the head is riding high – is it a bone loss issue, a ligament problem, or a combination?
It’s fundamentally about restoring the normal relationship between the humeral head and the glenoid. Think of it like a poorly fitted socket joint. We need to either reshape the ball, deepen the socket, or both. This ties directly into the broader field of shoulder arthroplasty (shoulder replacement) but often allows us to avoid or delay a full joint replacement, which is a huge win for the patient. We want to optimize natural tissues for as long as possible.
The first cornerstone is accurate diagnosis. MRI is critical, but it’s not foolproof. You need a surgeon experienced in reading these scans, looking for specific patterns of bone loss and cartilage damage. The second is meticulous surgical technique. Whether you’re performing a Latarjet procedure (bone block transfer), a remplissage (soft tissue reconstruction), or a glenoid labrum repair, precision is paramount. Small errors can lead to persistent instability.
A third crucial aspect is rehabilitation. A poorly managed rehab can undo even the best surgery. We're talking about a carefully phased program, starting with gentle range of motion exercises and gradually progressing to strengthening and functional activities. Compliance from the patient is key here – they need to understand the importance of following the protocol.
Finally, ongoing monitoring is essential. We need to track patients long-term to assess the durability of the repair and identify any signs of recurrent instability. This isn’t a “fix it and forget it” situation. It requires a committed partnership between the surgeon, the therapist, and the patient.
Getting the diagnosis right is 90% of the battle. You can have the best surgical skills in the world, but if you’re operating on the wrong problem, you’re going to get a poor outcome. We’re looking beyond just a dislocation history. We need to assess the degree of bone loss on the glenoid side – is it significant enough to warrant a bone block procedure? We also need to evaluate the integrity of the labrum and the surrounding soft tissues. It's a comprehensive assessment.
Standard X-rays are a good starting point, but they only tell part of the story. MRI is essential for visualizing the soft tissues and identifying cartilage damage. But even MRI can be misleading. Dynamic MRI studies, where the shoulder is moved during the scan, can provide valuable information about joint stability. And sometimes, an arthroscopic examination – a minimally invasive procedure where a camera is inserted into the shoulder joint – is necessary to get a clear picture of what’s going on.
It's not just about what you see on the images, but how you interpret them. That’s where experience comes in. A seasoned surgeon can often identify subtle signs of instability that might be missed by someone less familiar with the nuances of shoulder pathology. We have to combine imaging with a thorough clinical exam—assessing range of motion, strength, and any pain provocation tests.
There's a toolbox of surgical options here. The Latarjet procedure, transferring a piece of bone from the coracoid process to the glenoid, is a workhorse, especially for significant bone loss. It's robust, but it can sometimes lead to complications like nonunion (the bone doesn't heal) or nerve injury. Remplissage, a soft tissue reconstruction, is less invasive and can be effective for smaller bone defects.
Then you have glenoid labrum repair, which aims to restore the stability of the shoulder by repairing a torn labrum. This is often combined with other procedures, like capsular shifts, to address underlying ligamentous laxity. There's also the option of bone grafting – using bone from another source to augment the glenoid. The choice of technique depends on the individual patient, the severity of the bone loss, and the surgeon’s preference.
You see the Latarjet procedure widely adopted in Europe and Asia. It’s a well-established technique with good long-term results. Remplissage is gaining popularity in North America, particularly among surgeons who prefer a less invasive approach. But the specific techniques used can vary depending on local preferences, available resources, and the training of the surgeons.
In resource-limited settings, the focus is often on simpler, more cost-effective procedures. Sometimes, that means prioritizing rehabilitation and conservative management. But even in those settings, access to accurate diagnosis and skilled surgeons is crucial. We’re seeing more collaboration between international orthopedic societies to share knowledge and best practices.
The goal of high riding humeral head treatment isn't just to relieve pain; it's to restore function and allow patients to return to their activities. A successful treatment can mean the difference between being able to play sports, work, and enjoy life without limitations, and living with chronic pain and disability. That’s a huge impact.
We're seeing patients return to overhead activities, like throwing, swimming, and tennis, with good results. But it’s not a guarantee. There's always a risk of recurrence, and patients need to be realistic about their expectations. Long-term, the key is adherence to a rehabilitation program and a commitment to maintaining shoulder health.
Beyond the physical benefits, there's a significant psychological impact. Being able to regain control of your shoulder and return to the activities you love can dramatically improve quality of life.
We're starting to see the use of augmented reality and virtual reality in surgical planning and training. This allows surgeons to visualize the anatomy and practice complex procedures in a simulated environment. It’s a game changer for training and precision.
Biologic approaches are also gaining traction. Things like platelet-rich plasma (PRP) and stem cell therapy are being investigated as ways to promote healing and regeneration of cartilage. The results are still preliminary, but the potential is exciting.
And then there’s the rise of personalized medicine. Using genetic information to predict a patient’s response to different treatments and tailor the surgical approach accordingly. We are looking at patient specific instrumentation for improved accuracy, and also at more advanced imaging modalities to better assess the quality of the bone and cartilage.
| Surgical Technique | Patient Compliance | Pre-operative Condition | Post-operative Rehabilitation |
|---|---|---|---|
| Latarjet Procedure | High (9/10) | Significant bone loss (7/10) | Strict protocol adherence (8/10) |
| Remplissage | Moderate (7/10) | Mild to moderate bone loss (6/10) | Moderate adherence (6/10) |
| Glenoid Labrum Repair | Moderate (6/10) | Intact glenoid (5/10) | Progressive program (7/10) |
| Bone Grafting | High (8/10) | Severe bone loss (9/10) | Delayed weight-bearing (5/10) |
| Capsular Shift | Low (5/10) | Ligamentous laxity (7/10) | Range-of-motion exercises (6/10) |
| Arthroscopic Stabilization | Moderate (7/10) | Minimal bone loss (5/10) | Early mobilization (8/10) |
Recovery varies, but generally expect 6-9 months to return to full activity. The initial phase (0-6 weeks) focuses on pain control and gentle range of motion. Then comes strengthening (6-16 weeks), and finally, a gradual return to sports or demanding activities (6-9 months). It's critical to follow the therapist's protocol—rushing things can lead to setbacks. We’ll closely monitor your progress and adjust the plan as needed.
A Bankart repair focuses on reattaching the torn labrum to the glenoid. It’s great for anterior instability, but less effective when there’s significant bone loss. A Latarjet, on the other hand, transfers bone from the coracoid process to the glenoid, creating a new bony block to prevent dislocations. It’s more robust for cases with significant bone deficiency but is a more invasive procedure.
Like any surgery, there are risks. These include infection, nerve injury, blood clots, and hardware failure. Specific to shoulder surgery, you can get stiffness, recurrent instability, or nonunion (if bone grafting is involved). We discuss these risks thoroughly before surgery and take precautions to minimize them.
Absolutely. Physical therapy is crucial. It's not optional. It helps restore range of motion, strengthen the muscles around the shoulder, and improve overall function. Without proper rehab, the surgery is much less likely to be successful. We work closely with therapists who specialize in shoulder rehabilitation.
In some cases, yes. Conservative treatment with physical therapy, activity modification, and pain management can be effective, particularly in mild cases or for patients who aren’t candidates for surgery. However, if conservative treatment fails, surgery is often the best option to prevent further damage and restore function.
With successful treatment and diligent rehabilitation, most patients can return to their desired activities. However, it’s important to understand that the shoulder may not be exactly the same as before. There may be some residual pain or limitations, especially with overhead activities. Continued maintenance exercises are key to preserving function long-term.
High riding humeral head treatment represents a significant advancement in managing shoulder instability. From precise diagnostics and tailored surgical techniques to dedicated rehabilitation protocols, a comprehensive approach is essential for optimal outcomes. The future promises even more innovative solutions, leveraging technology and a deeper understanding of biomechanics to restore function and improve quality of life for countless individuals.
The key takeaway is that early intervention and a collaborative partnership between surgeon, therapist, and patient are paramount. If you suspect you may have a high riding humeral head, don’t delay seeking expert evaluation. Don't let shoulder pain sideline you. To learn more about our specialized treatment options and find a qualified surgeon, visit our website: high riding humeral head treatment.