- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
Comprehensive Guide to Lateral Hip Dislocation Diagnosis and Effective Treatment
Understanding Lateral Hip Dislocation: Causes, Symptoms & Treatment
A lateral hip dislocation occurs when the head of the femur (thigh bone) moves out of the acetabulum (hip socket) in a sideways direction. This is a serious injury, often resulting from high-energy trauma. Prompt diagnosis and appropriate treatment are crucial to minimize long-term complications. This article will delve into the causes, symptoms, diagnostic approaches, and available treatment options for lateral hip dislocations, offering a comprehensive overview for patients and healthcare professionals. Understanding the complexities of this injury is the first step toward effective management.
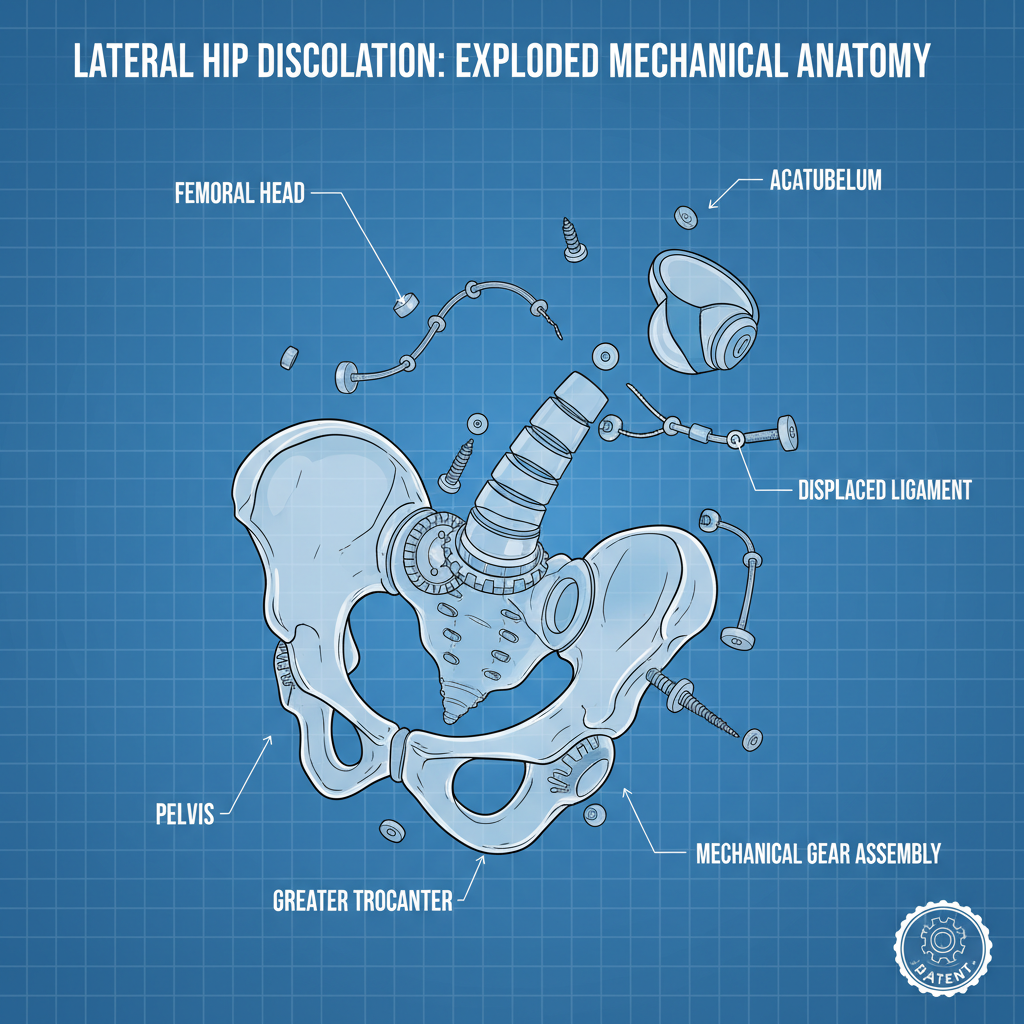
Causes of Lateral Hip Dislocation
The most common cause of a lateral hip dislocation is typically a high-impact event. This frequently occurs in motor vehicle accidents, particularly during pedestrian or motorcycle collisions. Falls from significant heights, sports-related injuries (especially contact sports), and violent trauma can also lead to this type of dislocation. In rare cases, underlying hip abnormalities or weakness in the surrounding musculature can predispose an individual to a dislocation with less severe trauma. It's important to note that the mechanism of injury often determines the direction of the dislocation – lateral, posterior, or anterior.
Key Takeaway: High-energy trauma is the primary culprit in most cases of lateral hip dislocation. Prompt medical evaluation is essential.
Recognizing the Symptoms of a Lateral Hip Dislocation
Symptoms of a lateral hip dislocation are typically dramatic and immediate. Intense pain in the hip and groin is a hallmark symptom. The affected leg will often appear shortened and externally rotated (turned outwards). Patients are usually unable to bear weight on the injured leg and may experience significant difficulty moving it. There might be visible deformity around the hip joint. Neurological symptoms, such as numbness or tingling in the leg and foot, can occur if nerves are compressed or damaged. A thorough physical examination is essential to assess the extent of the injury.
Common Symptoms:
• Intense hip and groin pain
• Leg shortening
• External rotation of the leg
• Inability to bear weight
• Possible neurological symptoms
Diagnosis of Lateral Hip Dislocation: Imaging & Assessment
Diagnosis typically begins with a clinical examination, focusing on the characteristic signs and symptoms. However, imaging studies are crucial to confirm the dislocation and assess for associated injuries. X-rays are the primary diagnostic tool, clearly revealing the displaced femoral head. A Computed Tomography (CT) scan may be necessary to provide more detailed views of the hip joint and identify any subtle fractures. Magnetic Resonance Imaging (MRI) can help evaluate soft tissue damage, such as labral tears or ligament injuries, which frequently accompany hip dislocations. Neurovascular assessment is essential to rule out any damage to nerves or blood vessels.
Treatment Options for Lateral Hip Dislocation: From Reduction to Rehabilitation
The primary goal of treatment is to restore the femoral head to its proper position within the acetabulum – a process called reduction. This is often performed under sedation or general anesthesia, as it can be quite painful. Following reduction, the hip is typically immobilized with a traction splint or cast to allow for healing. Surgical intervention may be necessary if there are associated fractures or significant soft tissue damage. Rehabilitation plays a critical role in restoring hip function and preventing long-term complications. This involves a gradual progression of exercises focusing on range of motion, strength, and proprioception. Rays Casting specializes in providing advanced immobilization solutions to support the healing process.
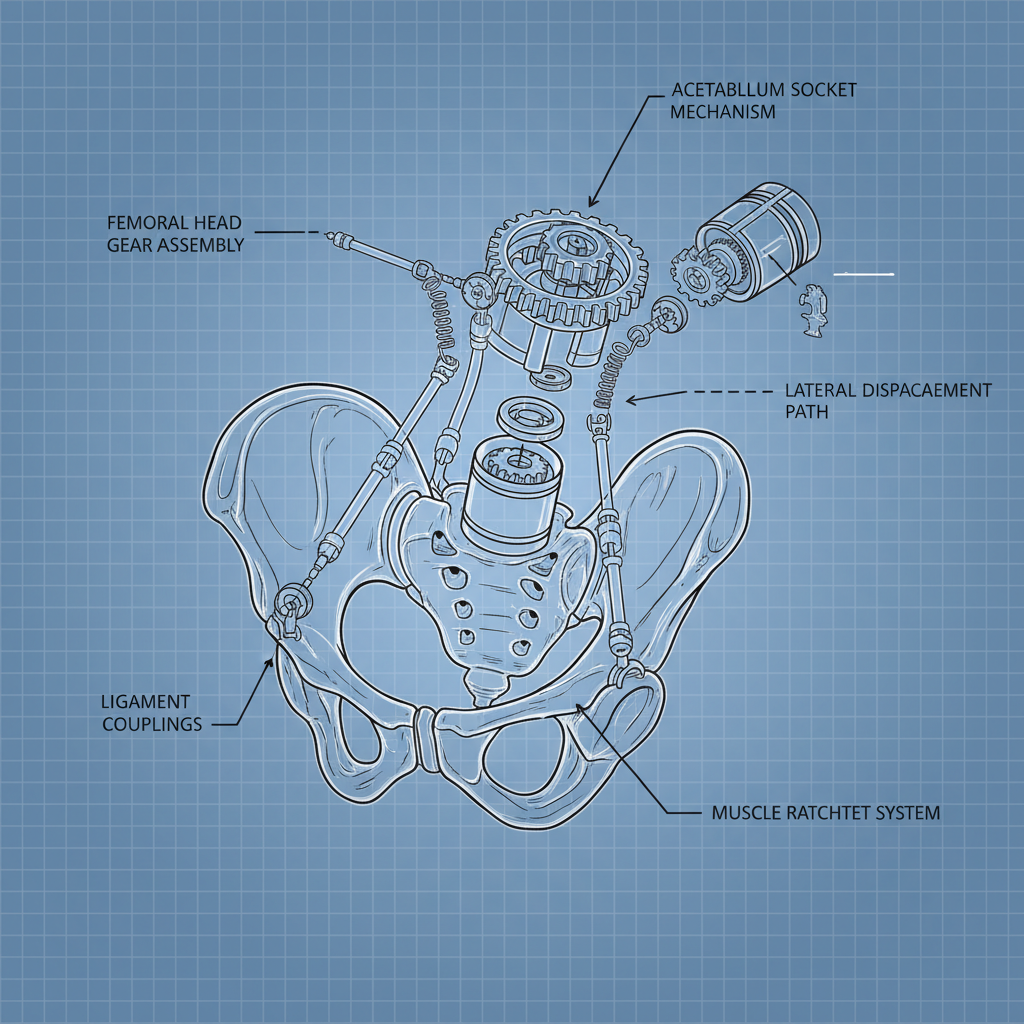
Long-Term Outlook & Potential Complications
While most patients experience a good recovery following a lateral hip dislocation, there are potential long-term complications. These can include avascular necrosis (AVN) of the femoral head, post-traumatic arthritis, and chronic hip instability. Early diagnosis, appropriate treatment, and diligent rehabilitation are vital to minimize these risks. Regular follow-up with an orthopedic specialist is recommended to monitor hip function and address any concerns.
Conclusion
A lateral hip dislocation is a serious injury requiring immediate medical attention. Understanding the causes, symptoms, and treatment options is crucial for optimal recovery. By seeking prompt care and adhering to a comprehensive rehabilitation program, patients can significantly improve their chances of regaining full hip function and returning to their desired activities.
Frequently Asked Questions (FAQs)
How long does it typically take to recover from a lateral hip dislocation?
Recovery time varies depending on the severity of the dislocation, the presence of associated injuries, and individual patient factors. Generally, initial immobilization lasts for several weeks, followed by a gradual rehabilitation program that can extend for several months. Full return to athletic activities may take 6-12 months or longer. Consistent adherence to the rehabilitation protocol is crucial for optimal outcomes.
What is the risk of developing arthritis after a hip dislocation?
The risk of developing post-traumatic arthritis following a hip dislocation is significant, estimated to be between 20-50%. The damage to the articular cartilage and labrum during the dislocation process can accelerate the degenerative changes within the joint. Maintaining a healthy weight, engaging in low-impact exercise, and potentially receiving preventative treatments (such as viscosupplementation) can help mitigate this risk.
Are there any preventative measures I can take to reduce my risk of hip dislocation?
While not all dislocations are preventable, strengthening the muscles surrounding the hip joint can improve stability and reduce the risk. This includes exercises targeting the glutes, hip flexors, and core muscles. Practicing proper form during athletic activities and avoiding high-risk behaviors (such as walking on icy surfaces) can also help. Addressing any underlying hip abnormalities or weaknesses is also important.
When should I seek immediate medical attention after a suspected hip dislocation?
Seek immediate medical attention if you experience sudden, severe pain in your hip, especially after a traumatic event. Other signs that warrant immediate care include inability to bear weight, visible deformity around the hip, and numbness or tingling in your leg or foot. Do not attempt to self-treat a suspected hip dislocation, as this can cause further damage.
Get a Custom Solution!
Contact Us To Provide You With More Professional Services