- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
The humeral head, a critical component of the shoulder joint, plays a pivotal role in a vast range of upper limb movements. Understanding its function is paramount not only in orthopedic surgery and rehabilitation but also in advancing the design and manufacture of high-precision medical implants. The increasing demand for shoulder arthroplasty, driven by an aging global population and heightened activity levels, underscores the significance of optimizing humeral head replacements and ensuring their long-term biomechanical compatibility. humeral head function is a cornerstone of successful shoulder restoration.
Globally, the incidence of shoulder pain and dysfunction is rising, presenting a substantial economic and healthcare burden. According to the World Health Organization, musculoskeletal conditions are a leading cause of disability worldwide, impacting quality of life and productivity. The precision manufacturing of components affecting humeral head function directly addresses this challenge by offering improved patient outcomes and reducing the need for revision surgeries. Furthermore, advancements in materials science and implant design are continually refining our understanding and application of humeral head function.
Within the specialized equipment manufacturing sector—specifically, medical device production—the accurate reproduction and reliable performance of the humeral head is fundamental. This necessitates a deep understanding of its biomechanics, material properties, and interaction with surrounding tissues. Improving humeral head function through precise engineering contributes to enhanced prosthetic joint functionality and patient satisfaction, solidifying its importance in modern healthcare.

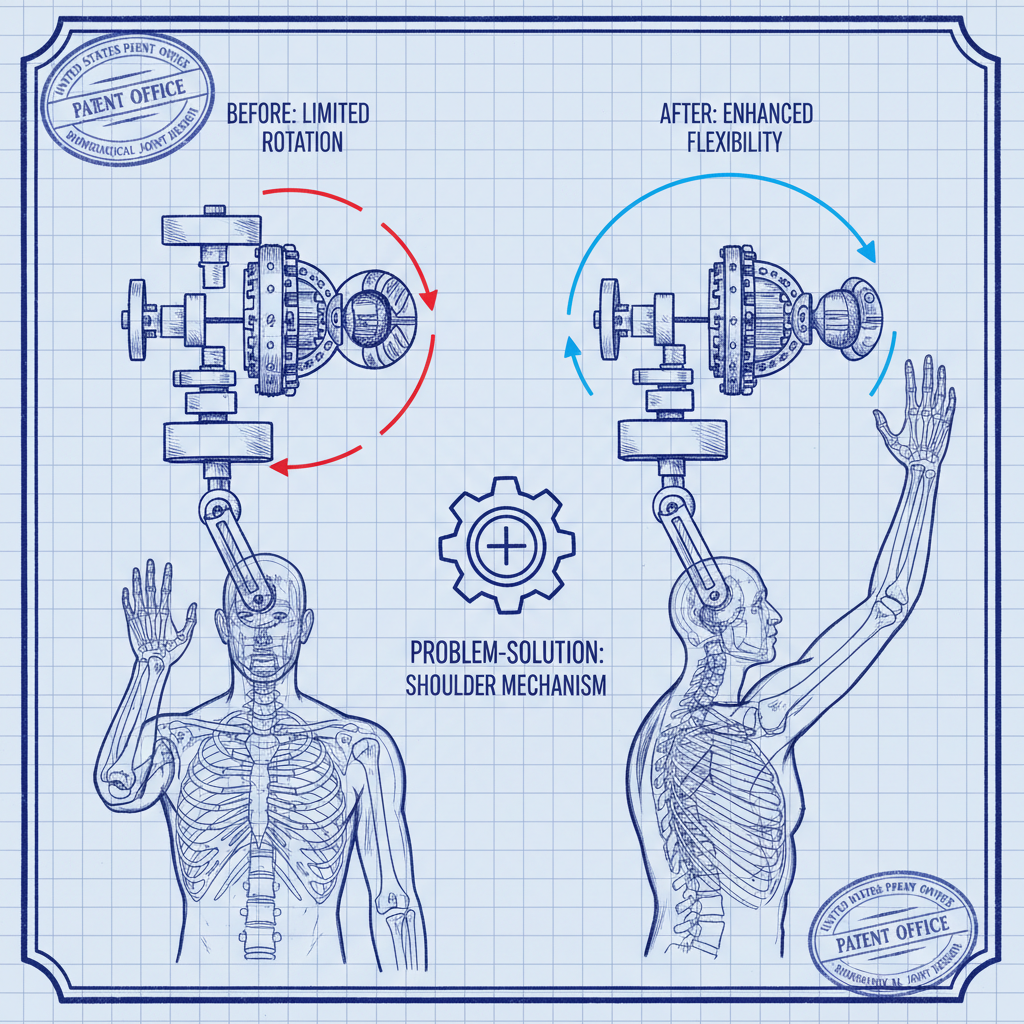
The successful execution of upper limb activities – from simple reaching to complex manipulations – fundamentally relies on the proper function of the humeral head. Its smooth articulation within the glenoid fossa is critical for maintaining a full range of motion and minimizing the risk of impingement or instability. Deficiencies in humeral head function can lead to debilitating pain and limited mobility, significantly affecting a patient’s quality of life.
From a manufacturing standpoint, replicating the natural geometry and biomechanical properties of the humeral head is a complex engineering challenge. Achieving this requires advanced techniques in material science, precision machining, and surface finishing to ensure long-term durability and optimal performance within the shoulder joint.
Humeral head function is best understood as a dynamic interplay between anatomy, biomechanics, and physiology. The humeral head isn’t simply a spherical cap; its subtle contours, variations in cartilage thickness, and connection to the surrounding rotator cuff muscles all contribute to its unique capabilities. These characteristics ensure efficient force transmission and stable shoulder movement throughout a wide arc of motion.
In the context of orthopedic implant design, mimicking this natural complexity is crucial. Implant materials must exhibit biocompatibility, wear resistance, and appropriate mechanical properties to avoid adverse reactions and ensure long-term stability. Furthermore, the precise positioning and alignment of the prosthetic humeral head are paramount to restoring optimal shoulder biomechanics and preventing complications.
Beyond the biomechanical considerations, understanding the physiological response to a prosthetic humeral head is essential. The body's reaction to the implant material, including bone ingrowth and soft tissue adaptation, influences the long-term success of the arthroplasty procedure and the restoration of humeral head function.
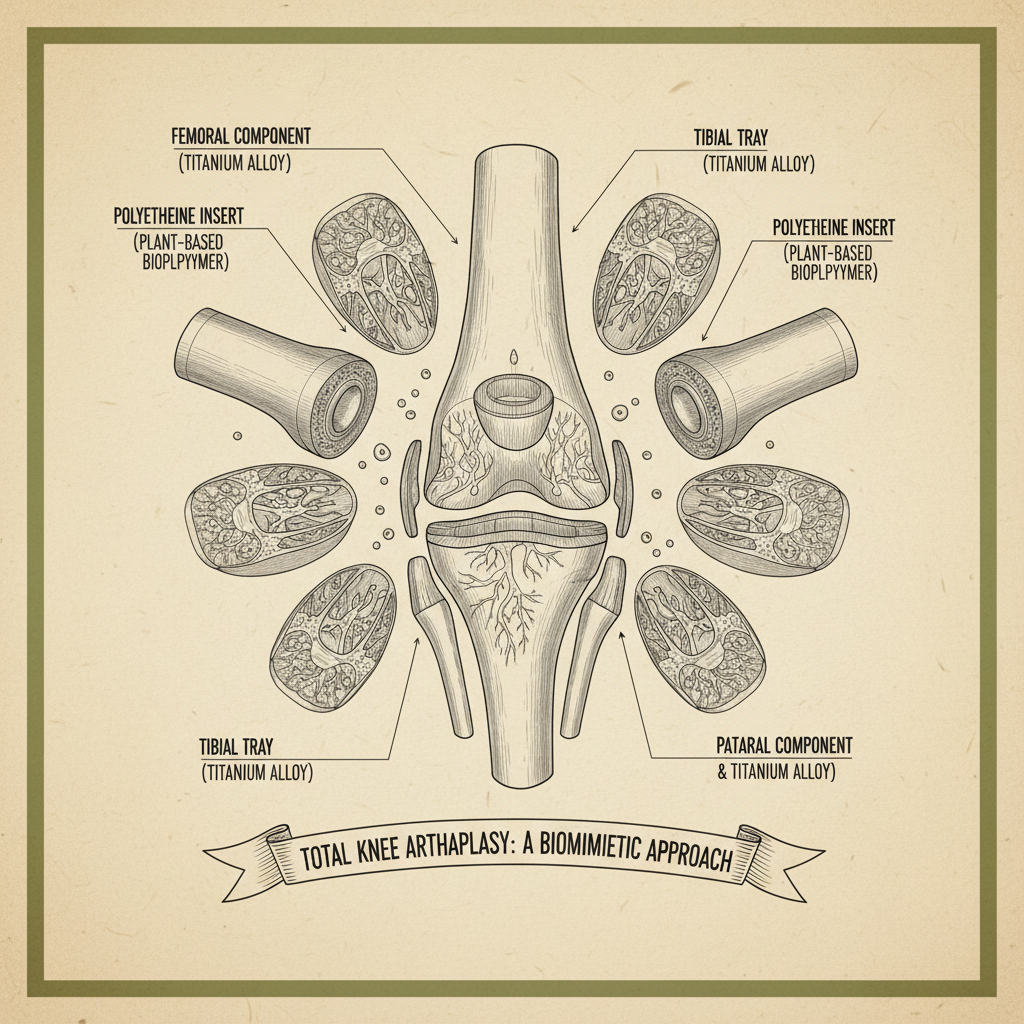
Several key components contribute to optimal humeral head function. First, congruity – the degree of fit between the humeral head and glenoid fossa – is critical for stability and minimizing wear. Second, articular cartilage provides a low-friction surface that facilitates smooth movement. Third, the rotator cuff muscles dynamically stabilize the shoulder joint and control movement patterns.
Fourth, bone density around the humeral head and glenoid fossa provides a solid foundation for implant fixation. Fifth, neuromuscular control allows for coordinated and precise movements. Finally, proprioception – the sense of joint position – provides feedback to the brain, enabling accurate and controlled movements. Each of these components must function in harmony to achieve optimal shoulder mechanics and restore full humeral head function.
Maintaining these components is crucial not just in healthy shoulders, but also in the design and implementation of artificial replacements. Understanding how each aspect impacts the overall function allows for targeted improvements in implant design and surgical techniques.
The principles of humeral head function are universally applicable, impacting orthopedic practices across the globe. From North America and Europe to Asia and Australia, shoulder arthroplasty is a common procedure for treating degenerative joint disease, rotator cuff tears, and traumatic injuries. The demand for high-quality shoulder implants is steadily increasing in emerging markets as healthcare access improves and populations age.
In specialized rehabilitation centers worldwide, therapists utilize exercises designed to restore optimal humeral head function following surgery or injury. These programs focus on strengthening the rotator cuff muscles, improving range of motion, and restoring neuromuscular control. Furthermore, advancements in surgical techniques, such as reverse total shoulder arthroplasty, are expanding the treatment options available for patients with complex shoulder pathology.
The development of advanced imaging technologies, such as MRI and CT scans, provides clinicians with detailed insights into humeral head function and assists in accurate diagnosis and treatment planning.
Optimizing humeral head function yields numerous benefits, ranging from improved patient outcomes to reduced healthcare costs. By restoring pain-free motion and enhancing upper limb functionality, patients can return to their daily activities with greater ease and confidence. This translates to increased productivity, improved quality of life, and reduced reliance on pain medication.
From a healthcare system perspective, successful shoulder arthroplasty procedures minimize the need for revision surgeries, which are often more complex and costly. Durable implants designed to preserve optimal humeral head function contribute to long-term patient satisfaction and reduced economic burden.
The future of humeral head function lies in the integration of advanced technologies and materials. Research into personalized implants, tailored to the unique anatomy of each patient, is gaining momentum. Additive manufacturing (3D printing) offers the potential to create customized humeral head replacements with complex geometries and optimized biomechanical properties.
Furthermore, the development of biocompatible coatings that promote bone ingrowth and reduce wear is crucial for enhancing implant longevity. Robotic-assisted surgery and augmented reality are also poised to revolutionize shoulder arthroplasty, allowing surgeons to perform procedures with greater precision and accuracy.
Despite significant advancements, challenges remain in achieving ideal humeral head function. Implant loosening, wear debris, and rotator cuff complications are potential long-term issues that require ongoing research and innovation. The variability in patient anatomy and surgical technique also poses a challenge to achieving consistent outcomes.
Addressing these challenges requires a multidisciplinary approach involving surgeons, engineers, materials scientists, and rehabilitation specialists. Developing advanced implant materials with improved wear resistance, optimizing surgical techniques to minimize soft tissue damage, and implementing personalized rehabilitation programs are all crucial steps towards achieving consistently successful shoulder arthroplasty outcomes.
Furthermore, continued investment in research and development is essential to unravel the complex interplay between implant design, biomechanics, and biological response, ultimately leading to the restoration of optimal humeral head function.
| Implant Material | Surgical Technique | Post-Operative Rehabilitation | Patient Specific Anatomy |
|---|---|---|---|
| Cobalt-Chromium Alloys | Minimally Invasive Approach | Early Range of Motion Exercises | Glenoid Morphology |
| Titanium Alloys | Precise Implant Positioning | Rotator Cuff Strengthening | Humeral Head Offset |
| Polyethylene Bearings | Bone Preservation Techniques | Proprioceptive Training | Arm Length Discrepancy |
| Ceramic Components | Rotator Cuff Repair Integration | Scapular Stabilization Exercises | Shoulder Instability History |
| Bioactive Coatings | Computer-Assisted Navigation | Gradual Return to Activities | Individual Activity Level |
| Hydroxyapatite | Suture Anchoring Techniques | Pain Management Protocol | Pre-existing Medical Conditions |
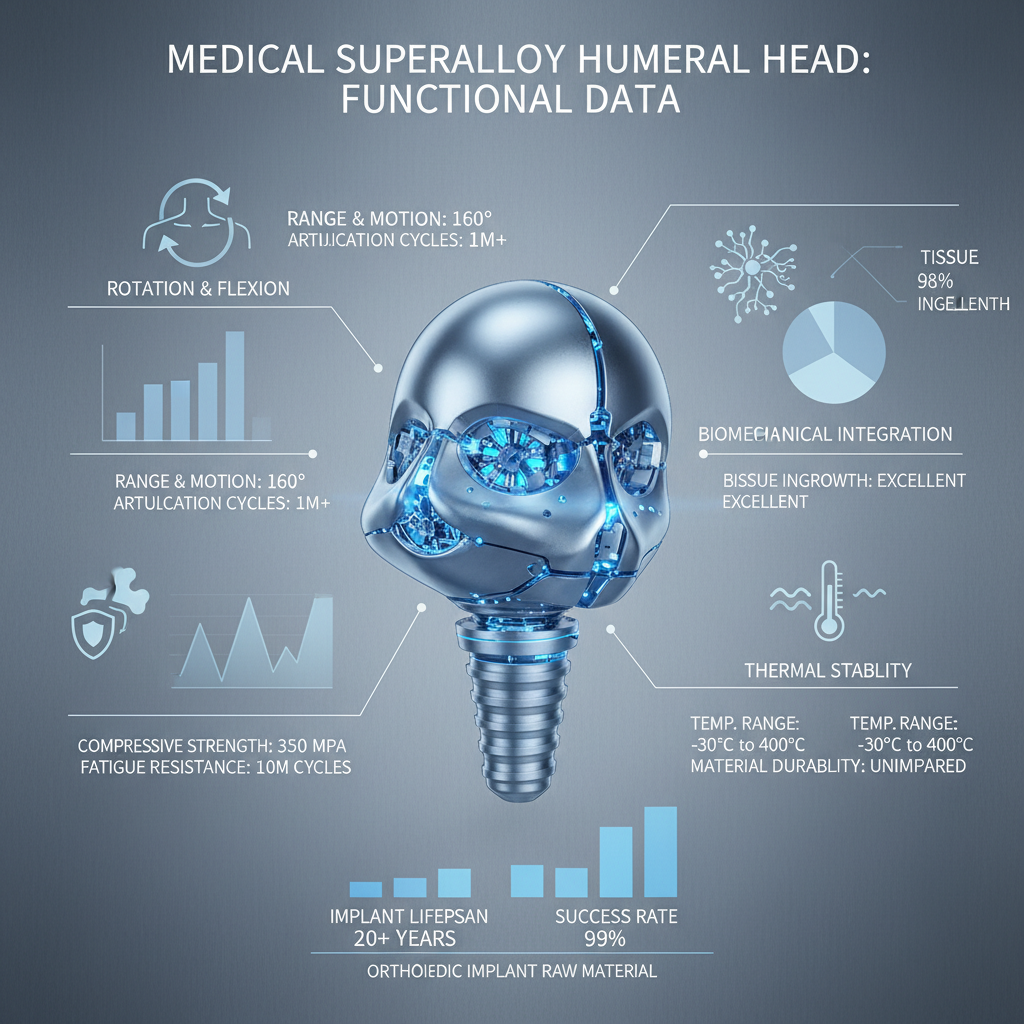
Following shoulder replacement aimed at restoring humeral head function, patients generally expect to regain a functional range of motion, typically achieving around 120-150 degrees of forward flexion, 45-60 degrees of external rotation, and adequate internal rotation for activities of daily living. This varies depending on individual factors and rehabilitation progress.
Improvements in humeral head function are usually noticeable within the first few weeks post-surgery, with continued gains over the following 6-12 months. Significant progress is often seen during the initial rehabilitation phase, focused on regaining range of motion and strengthening the surrounding muscles. The full benefits of restored function typically materialize with consistent rehabilitation efforts.
While shoulder replacement is generally safe, potential risks include infection, blood clots, nerve damage, implant loosening, and rotator cuff complications. These risks are minimized through careful surgical planning, adherence to sterile techniques, and appropriate post-operative care. Discuss these risks thoroughly with your surgeon.
Rehabilitation is absolutely critical for optimizing humeral head function after surgery. A structured program, guided by a physical therapist, focuses on regaining range of motion, strengthening muscles, improving proprioception, and restoring functional activities. Consistent adherence to the rehabilitation protocol is essential for achieving the best possible outcome.
Non-surgical options for improving humeral head function include physical therapy, pain management techniques (such as injections), and lifestyle modifications. These approaches can be effective for managing mild to moderate shoulder pain and dysfunction, but may not be sufficient for severe cases requiring surgical intervention.
The quality of the shoulder implant is a significant factor in long-term humeral head function. Implants manufactured with high-quality materials, precise engineering, and rigorous quality control processes are more likely to withstand the stresses of daily use and provide durable, reliable performance. Selecting an experienced surgeon who uses reputable implant systems is crucial.
In conclusion, understanding and optimizing humeral head function is paramount in the field of orthopedic surgery and medical device manufacturing. From the intricacies of shoulder biomechanics to the advancements in implant design and surgical techniques, a multidisciplinary approach is essential for restoring pain-free motion and enhancing the quality of life for patients suffering from shoulder dysfunction. The ongoing research and innovation in this area promise even more effective solutions in the future.
Looking ahead, the integration of personalized medicine, advanced materials, and robotic-assisted surgery will revolutionize the field of shoulder arthroplasty. Continued investment in research and development, coupled with a commitment to patient-centered care, will ultimately lead to improved outcomes and a greater understanding of the complex interplay between anatomy, biomechanics, and humeral head function. For further information and exploration of innovative solutions, visit our website: www.rays-casting.com