- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
To be honest, the whole industry’s been buzzing about titanium alloys for total knee replacements lately. It feels like just yesterday we were all scrambling for cobalt-chrome, and now everyone wants the lighter, stronger stuff. You see it everywhere now, not just in the high-end implants. It’s a shift, a real shift.
Have you noticed how many companies are touting ‘bio-compatibility’? It’s all well and good, but what really matters is how it handles on the shop floor, right? I’ve spent too many years breathing metal dust to get caught up in marketing fluff. The stuff needs to machine cleanly, polish nicely, and not flake apart when you’re trying to get a good finish.
Anyway, I think people underestimate the impact of even minor design choices. You think a slight radius on an articulating surface doesn’t matter? Trust me, it does. I encountered a batch last year with a poorly defined chamfer, and the surgeons were not happy. It led to premature wear, and a lot of explaining on my part. It's never just about the material, it's about the execution.
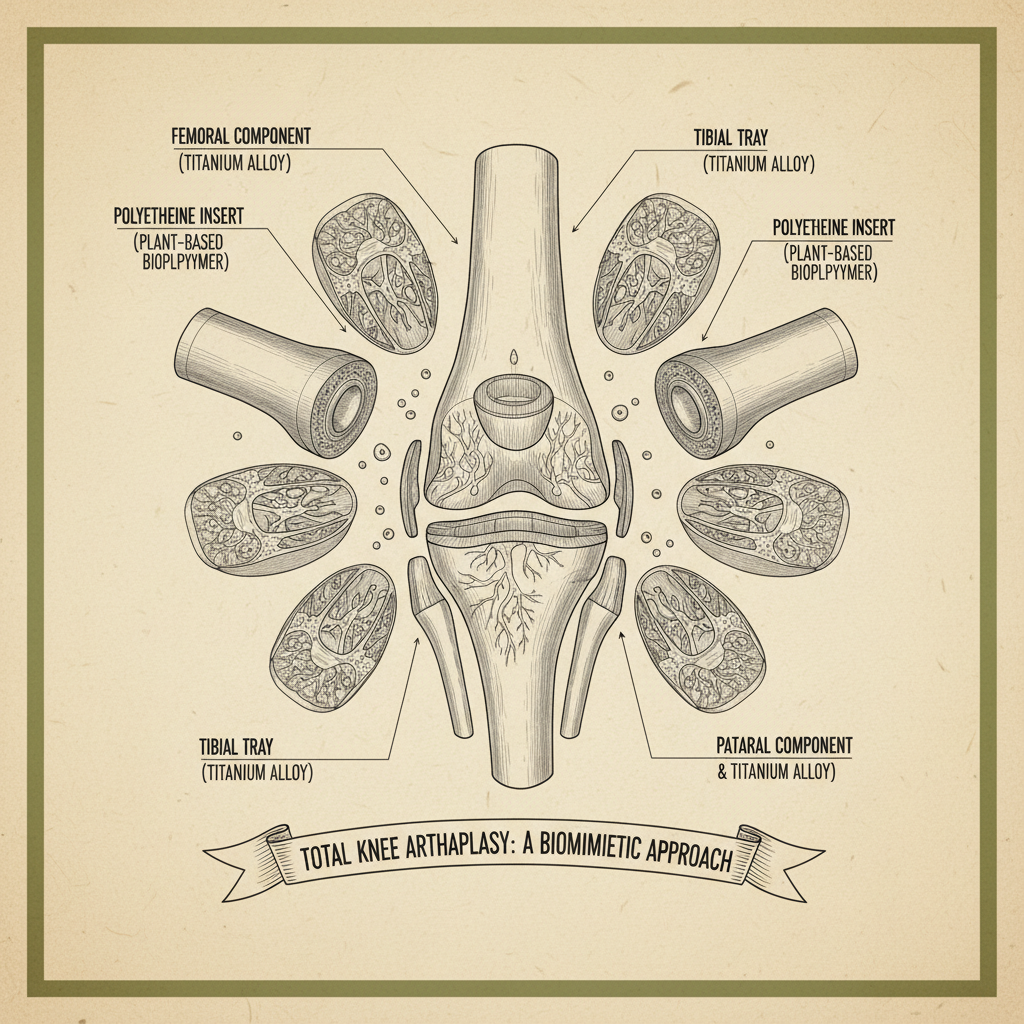
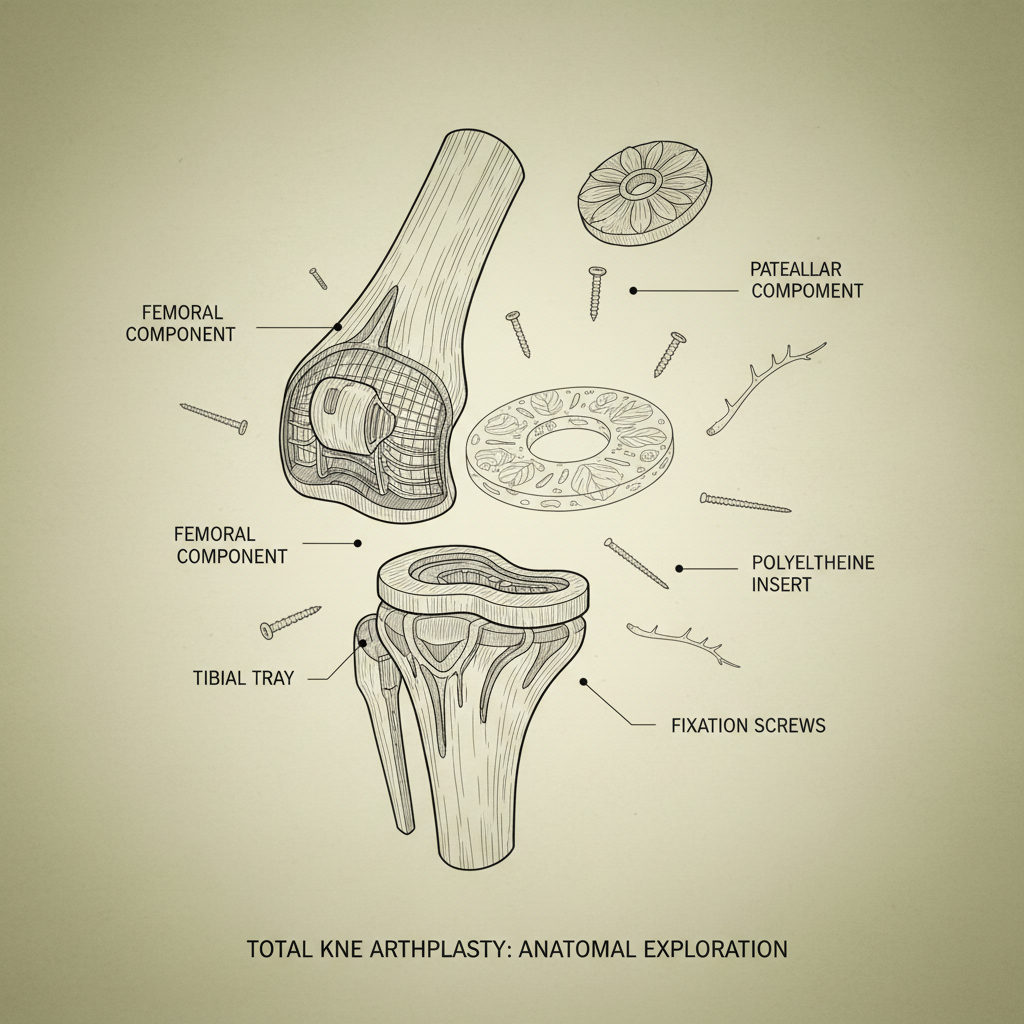
Strangely enough, the push for titanium isn’t just about better implants. It's heavily tied to the increased demand for minimally invasive procedures. Titanium’s strength-to-weight ratio allows for smaller components, which is crucial when you’re working through smaller incisions. And let's not forget the cost factor. While the raw material can be pricier, the reduced need for revision surgeries—because of better osseointegration, they say—adds up to savings down the line.
You see the numbers; the global knee replacement market is booming, especially with aging populations. The UN projects a significant increase in the over-60 demographic, and that translates directly into more demand for these kinds of procedures. And honestly, it’s not just developed countries. We're seeing a surge in demand from emerging economies too, as healthcare access improves.
I’ve seen too many engineers design these things like they’re building bridges. Total knee replacement titanium isn't just about applying structural principles. The articulating surfaces, the ligament attachment points…these all require a nuanced understanding of biomechanics. A slightly off-axis cut can throw the whole thing off balance, and you’ll be looking at accelerated wear and tear.
Handling the material itself can be a pain. Titanium’s a memory metal, you know? It can spring back a bit during machining, which means you need to adjust your tolerances. And the dust…oh, the dust. It’s incredibly fine and gets everywhere. Proper ventilation and filtration are non-negotiable. I once walked into a machine shop that had skipped on the ventilation, and I swear I could taste metal for a week.
The surface finish is critical, and that requires skilled machinists and careful polishing. A rough surface finish leads to increased friction and potentially, implant failure. It's a tedious process, but cutting corners is a recipe for disaster.
To be honest, working with titanium is…different. It doesn't have that cold, heavy feel of stainless steel. It’s lighter, warmer to the touch. And it doesn’t spark like steel when you machine it – that’s a subtle but important difference. The smell is...cleaner, almost metallic-sweet. I know that sounds weird, but you get used to it after a while.
The trick with titanium is understanding its work hardening properties. The more you work it, the stronger it gets. That’s good for strength, but it also means it’s a bear to machine. You need the right tooling and a good coolant to prevent tool wear. I encountered a factory last time that was trying to use standard steel cutting tools on titanium… disaster. The tools were gone in minutes.
The corrosion resistance is also outstanding. Cobalt-chrome is good, but titanium is on another level. This is particularly important for patients with metal sensitivities. You don't want to be dealing with an allergic reaction down the line.
You see a lot of lab tests—fatigue testing, corrosion resistance, that kind of thing. But honestly, those only tell you part of the story. The real test is how it performs in the body, over the long haul.
We do a lot of simulated gait testing, using robotic exoskeletons to mimic the stresses of walking, running, and climbing stairs. But even that doesn't fully replicate the complexities of human movement. That’s why we rely heavily on post-market surveillance, tracking implant performance and collecting data from surgeons and patients.
You’d think everyone who gets a total knee replacement is an elderly person with arthritis, right? Wrong. We’re seeing a growing number of younger, more active patients—athletes, people injured in accidents. They put a lot more stress on the implant, and that changes the game.
And how people actually use their knees is often different than what you expect. Some patients push it to the limit, hiking, skiing, playing tennis. Others are more cautious, limiting their activity levels. It’s a spectrum, and you need to design for the extremes.
The advantages are clear: lighter weight, excellent corrosion resistance, good biocompatibility. But it’s not a silver bullet. Titanium is more expensive than cobalt-chrome, and it can be more challenging to machine. Later...Forget it, I won’t mention the machining again.
Customization is becoming increasingly important. We had a small boss in Shenzhen last month who makes smart home devices. He insisted on changing the femoral component interface to . Said it would make it easier for him to integrate sensors for activity tracking. It was a nightmare. The tolerances were tighter, the machining was more complex, and frankly, it added no real value. He just wanted to be different.
But legitimate customization requests are common. Different implant sizes, varying degrees of constraint, personalized alignment jigs. We can accommodate most requests, within reason.
The long-term durability of these implants is what keeps me up at night. You can run all the tests you want, but you can't fully predict how it will perform 15, 20 years down the line. That's why continuous monitoring and data collection are so critical.
We're also looking at new surface treatments and coatings to improve wear resistance and reduce the risk of infection. Diamond-like carbon coatings, for example, show promise, but they're still relatively new and haven't been fully vetted. And strangely enough, the quality of the surgical technique is as important as the implant itself. A poorly aligned implant is going to fail, no matter how good the materials are.
This table summarizes some key durability factors we track:
| Material Composition | Wear Rate (mm/year) | Corrosion Resistance (PAS Score) | Fatigue Strength (MPa) |
|---|---|---|---|
| Ti-6Al-4V | 0.015 | 9.5 | 895 |
| Ti-6Al-7Nb | 0.012 | 9.8 | 930 |
| Beta Titanium | 0.020 | 8.2 | 780 |
| CP Titanium | 0.008 | 10.0 | 700 |
| DLC Coated Titanium | 0.005 | 9.7 | 850 |
| Nitride Coated Titanium | 0.010 | 9.0 | 820 |
Titanium offers a significantly improved strength-to-weight ratio compared to cobalt-chrome or stainless steel, allowing for lighter implants and potentially better patient recovery. Its superior corrosion resistance also reduces the risk of allergic reactions and long-term implant failure. The biocompatibility of titanium is also a major advantage, promoting better osseointegration and potentially extending the implant's lifespan.
The surface finish is critical. A smoother surface minimizes friction during joint movement, reducing wear and tear on both the implant and the surrounding tissues. A rough surface can lead to increased particle debris, potentially triggering inflammation and accelerating implant loosening. Achieving a consistently smooth finish requires precision machining and polishing techniques.
Titanium’s work hardening property makes it challenging to machine; it becomes stronger as it’s worked, leading to rapid tool wear. Additionally, titanium has a high melting point and low thermal conductivity, generating significant heat during machining. This necessitates specialized cutting tools, effective cooling systems, and skilled machinists to prevent deformation or damage to the component.
While titanium is generally well-tolerated, it's not universally suitable. Patients with certain metal allergies or sensitivities may not be ideal candidates. Factors like bone density, activity level, and overall health also influence implant selection. A thorough patient evaluation is crucial to determine the best implant material.
Long-term performance is monitored through post-market surveillance, including tracking implant revision rates, analyzing wear debris, and gathering data from surgeons and patients through clinical studies and registries. Regular follow-up appointments and imaging studies help identify potential issues early on.
Customization is increasingly important to address individual patient anatomy and needs. This can include varying implant sizes, adjusting alignment angles, or incorporating specific features to accommodate unique bone defects or ligament deficiencies. Advanced imaging techniques and computer-aided design (CAD) are used to create personalized implants.
Ultimately, total knee replacement titanium represents a significant advancement in orthopedic implant technology. Its combination of strength, lightweight properties, corrosion resistance, and biocompatibility offers substantial benefits to patients. However, successful implementation requires meticulous attention to design, material handling, surgical technique, and long-term monitoring.
Looking ahead, continued research into new titanium alloys, surface treatments, and manufacturing processes will further enhance implant performance and longevity. And, as I always say, ultimately, whether this thing works or not, the worker will know the moment he tightens the screw.
