- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
You know, it's been a crazy year. Seems like everyone's talking about lightweighting these days, especially in knee replacements. Titanium alloys, of course, are the go-to, but it's not as simple as just saying "titanium." There’s a lot of nuance. Everyone wants a stronger, lighter implant, but they forget about manufacturability, and then you’re stuck with a design that looks great on paper but is a nightmare to actually make.
Honestly, I’ve seen so many designs come through where someone gets cute with the geometry, and then the machining costs skyrocket. It’s a balancing act, always. And the demand for custom solutions is up, too. People are realizing a one-size-fits-all approach doesn't always cut it.
I was at a factory in Changzhou last month, and they were telling me about the difficulty sourcing high-quality titanium sponge. It’s not just the price, it's the consistency. Different batches can have slightly different properties, which affects the final product. It’s a real headache for quality control.
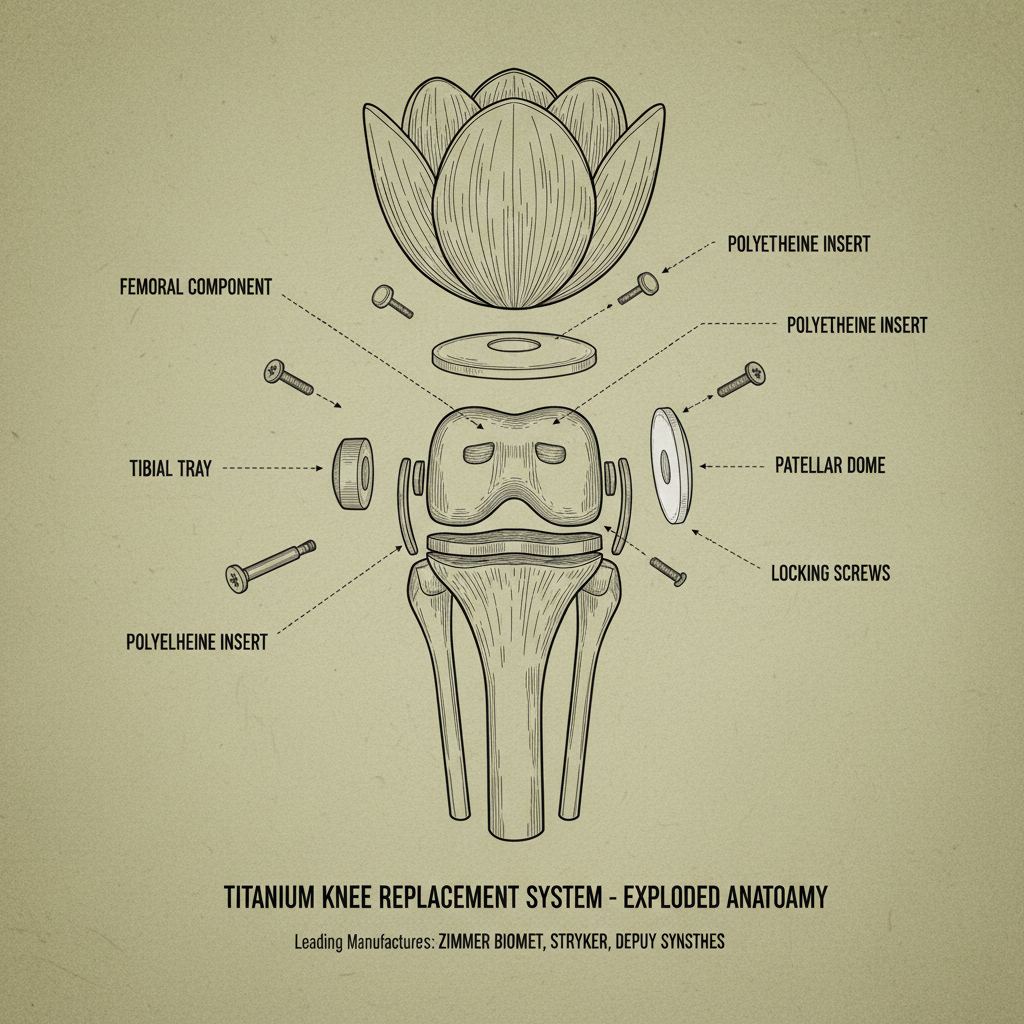
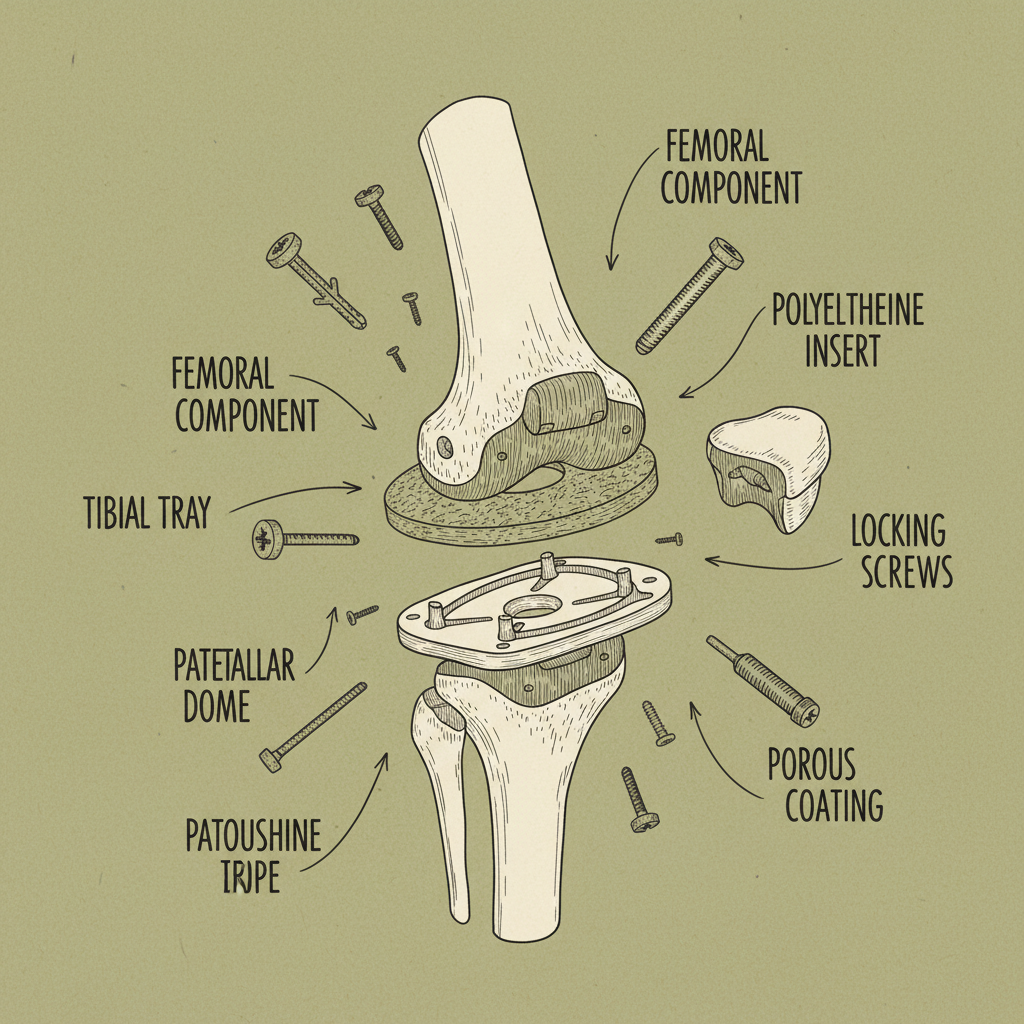
The market for titanium knee replacements is, well, it’s booming. Aging populations, increased activity levels – everyone wants to stay mobile longer. But it’s not just about demand; it's about patient expectations. They want something that feels right, lasts a long time, and doesn’t interfere with their lifestyle. And frankly, a lot of that comes down to the materials and the design. To be honest, the pressure to innovate is relentless.
We’re seeing a lot of companies focusing on porous titanium coatings to encourage bone ingrowth. That’s good, theoretically, but getting the porosity just right is tough. Too little, and the bone doesn’t integrate properly. Too much, and you compromise the structural integrity.
Have you noticed how many designs try to mimic the natural knee joint exactly? It looks good in the CAD model, but it ignores the realities of manufacturing and wear. Complex curves, tight tolerances… it all adds up to increased costs and potential failure points. Simplicity, often, is better.
And the screw holes! Oh, the screw holes. I encountered this at a factory in Suzhou last time. They were struggling with stress concentrations around the screw bosses. They’d designed it to look sleek, but it was inherently weak. You need to carefully consider the load paths and ensure adequate material support.
Also, everyone's obsessed with reducing the size of the implant, but they forget that surgeons need something they can reliably fixate. You can’t go too small, or you risk instability. It's a delicate balance.
It’s not just “titanium.” There’s Ti-6Al-4V, which is the workhorse, but then you have beta titanium alloys, which offer higher strength but are more difficult to work with. The feel is different, too. Ti-6Al-4V is… well, it feels like titanium. A bit cold, a bit rough. Beta titanium, it’s almost springy, almost… alive. Strangely, sometimes a surgeon can tell the difference just by handling it.
The surface treatment is crucial, too. We’re seeing a lot of plasma spraying, hydroxyapatite coatings, and now even bioactive glass coatings. The goal is to create a surface that encourages bone to grow onto the implant. It smells a little bit like burnt toast when they’re applying the coating, by the way. Not pleasant, but it means it’s working.
And don’t even get me started on the quality control of the raw materials. You need to be able to trace every batch of titanium sponge back to its source, and you need to verify its composition and purity.
Lab testing is fine, but it doesn’t tell the whole story. You need to simulate real-world conditions. We do fatigue testing, of course, cycling the implant through millions of loading cycles. But we also do impact testing, drop testing, and even corrosion testing in simulated body fluids.
We also work with surgeons to get feedback on the implants during cadaveric studies. They can tell you how it feels to insert, how easy it is to fixate, and whether it has any unexpected quirks. They are the ultimate validator. Anyway, I think that’s the most important part of the process.
Surgeons aren’t always going to follow the instructions to the letter. They’ll modify the technique, they’ll use different instruments, and they’ll adapt the implant to the patient’s anatomy. It's just what they do. You have to design for that variability.
I’ve seen surgeons use the implant as a lever to help with alignment, or they’ll use it to create a guide for bone cuts. It’s not what we intended, but it works for them. And ultimately, that’s what matters.
Titanium’s great, obviously. Lightweight, strong, biocompatible. But it's expensive, and it can be a pain to machine. And the finish… sometimes it can be a bit dull. It doesn’t have the same luster as, say, cobalt-chrome. But cobalt-chrome is heavier.
Customization is becoming a big thing. Surgeons want implants tailored to their patient's specific anatomy. We can do that with 3D printing, but it adds cost and complexity. But for a tricky case, it can be worth it. We had one case last year where a patient had a severely deformed knee, and a standard implant just wouldn’t fit. We 3D printed a custom implant, and it was a success.
Later... forget it, I won’t mention it, the cost of that one almost gave me a heart attack.
Last month, that small boss in Shenzhen who makes smart home devices – he's got a side hustle building medical components now – insisted on changing the interface to . Said it was “more modern.” I told him it was a terrible idea – surgeons are used to the standard locking mechanism, and they don’t want to mess around with fiddly connectors during surgery. He wouldn't listen.
He said it would "differentiate" his product. He even showed me a slick marketing video. Anyway, he went ahead with it, and the first surgeon who used it nearly dropped the implant. The connection wasn't secure enough. He called me, furious. We had to pull the whole batch and redesign the interface. It cost him a fortune.
It's a good reminder that in medical devices, functionality trumps innovation almost every time.
| Alloy Composition | Surface Roughness (Ra) | Porosity (%) | Tensile Strength (MPa) |
|---|---|---|---|
| Ti-6Al-4V ELI | 0.8 µm | 30-40% | 950 |
| Beta Titanium (Ti-13V-11Cr-3Al) | 1.2 µm | 20-30% | 1100 |
| CP Titanium (Grade 2) | 0.4 µm | 5-15% | 485 |
| Ti-6Al-4V with HA Coating | 1.0 µm | 45-55% | 900 |
| Beta Titanium with Bioactive Glass | 1.5 µm | 35-45% | 1050 |
| Custom Alloy (Ti-Zr-Nb) | 0.6 µm | 25-35% | 980 |
The lifespan of a titanium knee replacement varies, but generally, they’re designed to last 15-20 years or more. However, this depends heavily on patient activity level, weight, and overall health. We’ve seen some implants still functioning well after 25 years, but realistically, most patients will likely need a revision surgery at some point, especially if they're very active or experience significant weight gain.
Titanium implants are generally more expensive upfront than cobalt-chrome alloys due to the higher cost of the raw material and the more challenging machining processes. However, the longer-term benefits, like reduced risk of allergic reaction and potentially better osseointegration, can offset the initial cost. Plus, there’s the weight factor – lighter implants can be easier for patients to rehabilitate.
Manufacturers need to comply with ISO 13485 for quality management systems, and the implants themselves must meet the requirements of the relevant regulatory bodies – like the FDA in the US, or CE marking in Europe. They also need to demonstrate biocompatibility and undergo rigorous testing to ensure safety and efficacy. Audits are frequent, and the documentation requirements are… extensive.
Titanium is generally considered hypoallergenic, and true titanium allergies are rare. However, some titanium alloys contain vanadium, which can cause allergic reactions in a small percentage of patients. We carefully select our alloys to minimize the vanadium content, and we always conduct thorough pre-operative screening to identify potential sensitivities.
The manufacturing process is critical. Proper heat treatment, surface finishing, and quality control are essential to ensure the implant’s mechanical properties and resistance to corrosion. Any defects introduced during manufacturing can significantly shorten the implant’s lifespan. We use non-destructive testing methods – like X-ray and ultrasound – to detect any internal flaws.
There's a lot of research going into new titanium alloys with improved strength, fatigue resistance, and biocompatibility. Beta titanium alloys are gaining traction, and we're also exploring the use of titanium foams and porous structures to enhance bone ingrowth. Additive manufacturing (3D printing) is also opening up new possibilities for customized implant designs.
So, titanium knee replacements – they’re not just a piece of metal. They’re a complex combination of material science, engineering, and surgical expertise. The industry is pushing for lighter, stronger, more biocompatible implants, and customization is becoming increasingly important. But at the end of the day, it’s about restoring mobility and improving patients’ quality of life.
Ultimately, whether this thing works or not, the worker will know the moment he tightens the screw. That's all that really matters. If it feels solid, if it fits right, if it gives the surgeon confidence… then we’ve done our job. Visit our website at www.rays-casting.com to learn more about our titanium knee replacement solutions.
