- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
Type 3 acromioclavicular (AC) joint injuries represent a significant challenge in orthopedic medicine, impacting individuals across a wide spectrum of activities and age groups. These injuries, characterized by complete disruption of both the acromioclavicular and coracoclavicular ligaments, often result from high-energy trauma such as falls or direct blows to the shoulder. Understanding the nuances of type 3 acromioclavicular joint injury is crucial for appropriate diagnosis, treatment, and ultimately, restoring optimal shoulder function and quality of life for affected individuals.
The global relevance of AC joint injuries, specifically type 3, stems from the increasing participation in sports, recreational activities, and the aging population prone to falls. The incidence is estimated to be around 3.4 per 100,000 person-years, with a peak in young, active adults. While precise global statistics are difficult to obtain, the prevalence is consistently reported across developed nations, and likely underreported in developing regions due to limited access to healthcare and diagnostic facilities. Effective management strategies are vital to minimize long-term disability and associated healthcare costs.
A type 3 acromioclavicular joint injury is a complete dislocation of the AC joint, meaning the acromion (the bony tip of the shoulder blade) has separated significantly from the clavicle (collarbone). This separation involves tearing of all the ligaments that normally stabilize the AC joint, including the acromioclavicular and coracoclavicular ligaments. It’s more severe than types 1 and 2, and often requires surgical intervention to restore proper alignment and function. Addressing this injury promptly is paramount for individuals requiring full shoulder function in their daily lives or athletic pursuits.
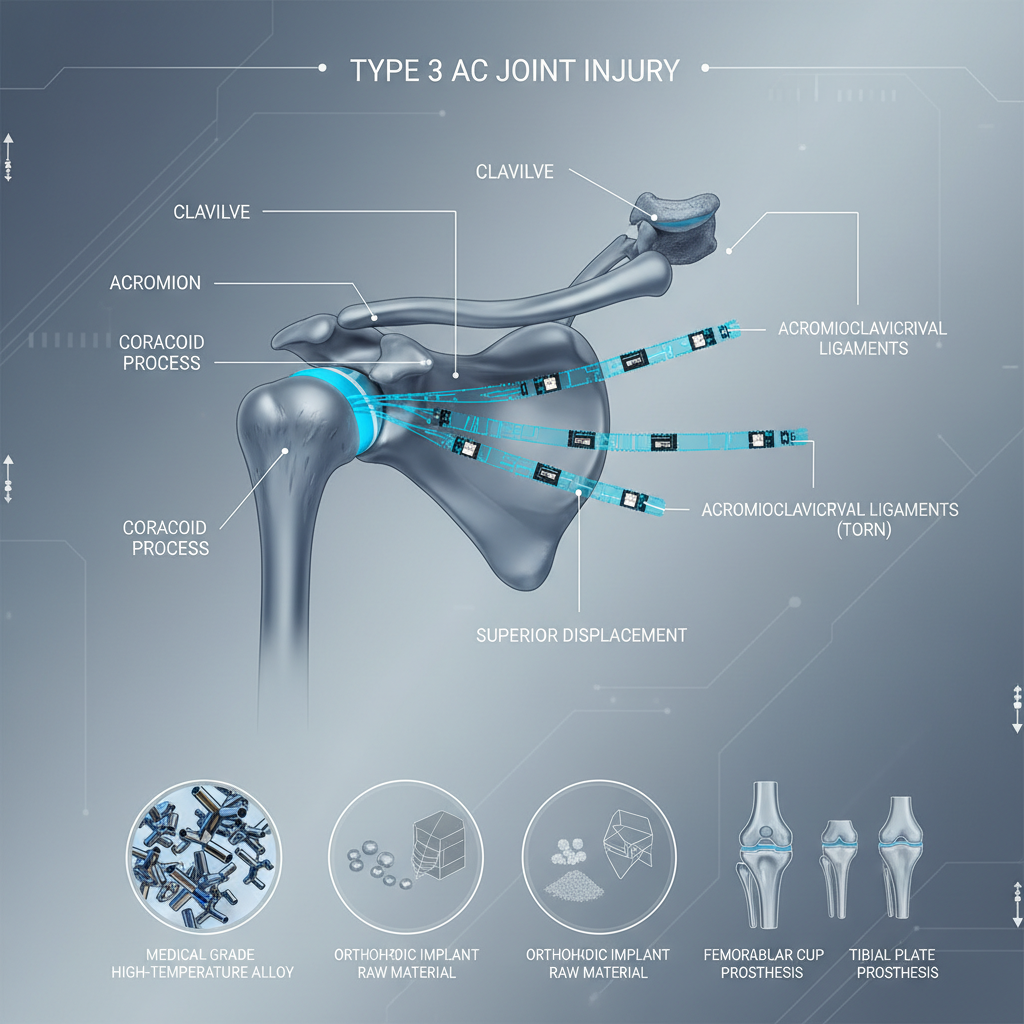

The underlying mechanism of a type 3 acromioclavicular joint injury typically involves a direct fall onto the shoulder, a forceful impact, or a collision. These forces overwhelm the stabilizing ligaments, resulting in complete separation of the AC joint. The severity of the injury correlates with the degree of displacement, with type 3 injuries exhibiting significant vertical displacement of the clavicle relative to the acromion. Accurate identification of the injury type is critical for appropriate treatment planning.
Distinguishing a type 3 acromioclavicular joint injury from less severe types (1 and 2) relies heavily on physical examination findings and radiographic imaging. Physical examination reveals obvious deformity, marked tenderness over the AC joint, and inability to bear weight across the arm. Radiographs confirm the complete disruption of the ligaments and demonstrate the characteristic upward displacement of the clavicle.
The Rockwood classification system is widely used to categorize AC joint injuries based on the degree of ligamentous damage and clavicular displacement. Type 3 injuries fall into a distinct category, signifying complete disruption of both the acromioclavicular and coracoclavicular ligaments. This complete disruption leads to substantial instability and noticeable deformity. The injury’s severity directly impacts the functional limitations experienced by the patient.
Compared to Type 1 and 2 injuries, a type 3 acromioclavicular joint injury involves significantly more ligamentous damage. Type 1 typically involves a sprain, while Type 2 involves a partial tear. These less severe injuries can often be managed conservatively, whereas type 3 injuries almost always require surgical intervention to restore proper anatomy and function. The decision for surgical versus conservative management depends on patient factors, activity level, and the degree of functional impairment.
Recognizing the distinction between injury types is crucial for informing patient expectations and guiding treatment decisions. Failing to recognize a type 3 injury and attempting conservative management can lead to chronic pain, instability, and diminished shoulder function. Conversely, appropriately diagnosing and addressing a type 3 injury allows for a targeted and effective treatment approach.
The acromioclavicular (AC) joint is formed by the articulation between the acromion process of the scapula and the distal end of the clavicle. This joint is stabilized by a complex network of ligaments, most notably the acromioclavicular ligament and the coracoclavicular ligaments (conoid and trapezoid). The coracoclavicular ligaments are particularly important in preventing vertical displacement of the clavicle.
In a type 3 acromioclavicular joint injury, all these ligaments are completely torn. This complete ligamentous disruption leads to significant instability and the characteristic upward and outward displacement of the clavicle. Understanding the anatomy and function of these ligaments is critical for comprehending the pathophysiology of the injury and selecting the appropriate surgical reconstruction technique.
The surrounding muscles, including the deltoid, trapezius, and rotator cuff muscles, also contribute to shoulder stability, but they cannot compensate for complete ligamentous disruption. These muscles may spasm in an attempt to stabilize the joint, contributing to pain and discomfort. Therefore, restoring ligamentous integrity is paramount for achieving long-term shoulder stability.
Diagnosing a type 3 acromioclavicular joint injury begins with a thorough physical examination, assessing for pain, deformity, and the ability to bear weight across the arm. The physical exam is often sufficient to strongly suspect a complete AC joint dislocation. However, radiographic imaging is essential to confirm the diagnosis and rule out associated fractures.
Standard anteroposterior (AP) radiographs, along with axillary views, are typically obtained. These images demonstrate the characteristic upward displacement of the clavicle. Stress views, where weight is applied to the arm, can further highlight the instability of the AC joint. In some cases, magnetic resonance imaging (MRI) may be used to evaluate the extent of ligamentous damage and assess for associated soft tissue injuries.
Type 3 acromioclavicular joint injuries affect a diverse patient population across all geographic regions. The most common demographic is young, active individuals participating in contact sports like football, hockey, and rugby, as well as high-impact recreational activities like skiing and snowboarding. However, falls from height can cause this injury in individuals of all ages.
In post-disaster relief operations, the incidence of type 3 AC joint injuries may increase due to traumatic events. Furthermore, the injury is observed in industrial settings involving heavy labor and potential for falls or direct impacts. Healthcare systems in regions with limited resources may face challenges in providing timely and appropriate care for these injuries.
Accurate and timely diagnosis of a type 3 acromioclavicular joint injury is essential for optimizing treatment outcomes. Early intervention, particularly surgical reconstruction, can prevent chronic pain, instability, and functional limitations. Restoring anatomical alignment allows patients to regain full range of motion, strength, and the ability to participate in desired activities.
Successful treatment leads to improved quality of life, reduced reliance on pain medication, and enhanced psychological well-being. For athletes, restoring shoulder function is critical for returning to their sport and maintaining their competitive edge. A well-managed type 3 AC joint injury minimizes the long-term impact on a patient’s physical and emotional health.
Moreover, accurate diagnosis and treatment contribute to cost savings by avoiding chronic care and potential disability. A proactive approach to injury management not only benefits the individual patient but also reduces the burden on healthcare systems.
Ongoing research is focused on refining surgical techniques for type 3 acromioclavicular joint injuries, exploring novel fixation methods and graft materials. Arthroscopic reconstruction is gaining popularity, offering a minimally invasive approach with potentially faster recovery times. Biologic augmentation, using techniques like platelet-rich plasma (PRP) or stem cells, is being investigated to enhance ligament healing.
The development of advanced imaging techniques, such as diffusion tensor imaging (DTI), may provide more detailed assessment of ligamentous damage. Artificial intelligence (AI) and machine learning algorithms could be used to analyze radiographic images and assist in diagnosis and treatment planning. Personalized rehabilitation protocols, tailored to individual patient needs and functional goals, are also emerging.
Furthermore, advancements in biomaterials are leading to the development of more durable and biocompatible implants for AC joint reconstruction. The goal is to optimize surgical outcomes, minimize complications, and restore long-term shoulder stability and function.
| Challenge | Current Limitations | Potential Solutions | Implementation Timeline |
|---|---|---|---|
| Ligament Reconstruction Failure | Suboptimal Graft Choice/Fixation | Utilize augmented grafts, improved fixation techniques | Short-term (1-3 years) |
| Postoperative Pain | Insufficient pain management protocols | Multimodal pain management, regional anesthesia | Immediate |
| Limited Range of Motion | Postoperative stiffness, scar tissue formation | Aggressive early rehabilitation, joint mobilization | Medium-term (3-6 months) |
| Difficulty in Diagnosis | Overlapping symptoms with other shoulder pathologies | Improved imaging protocols, clinical decision rules | Short-term (1-2 years) |
| Recurrent Instability | Inadequate ligament reconstruction, continued high-impact activity | Reinforced reconstruction, activity modification | Medium-term (6-12 months) |
| Cost of Treatment | Surgical intervention, rehabilitation, potential complications | Optimized surgical techniques, streamlined rehabilitation programs | Ongoing |
The recovery timeline for type 3 AC joint injury surgery is typically 6-12 months for a full return to activity. The initial phase (0-6 weeks) focuses on pain management and protected range of motion. Subsequent phases involve progressive strengthening exercises, gradually increasing range of motion, and functional activities. Return to sport is typically allowed around 6-12 months, depending on individual progress and the demands of the sport. Strict adherence to the rehabilitation protocol is crucial for optimal recovery.
While rare, non-operative treatment may be considered for select patients with type 3 AC joint injuries, particularly those with low functional demands and minimal symptoms. However, most patients experience persistent pain, instability, and reduced shoulder function with conservative management. Surgery is generally recommended to restore anatomical alignment and optimize long-term outcomes. The decision is made after a comprehensive evaluation considering patient factors and activity level.
Potential complications include infection, nerve injury, hardware failure, and persistent pain. Stiffness and limited range of motion are also relatively common, requiring dedicated rehabilitation. Recurrent instability, although less frequent, can occur if the reconstruction fails. Careful surgical technique, appropriate postoperative management, and adherence to rehabilitation protocols can minimize the risk of these complications.
The choice of graft material is a critical factor in AC joint reconstruction. Options include autografts (tissue taken from the patient’s own body) and allografts (tissue from a donor). Autografts generally have better integration and lower risk of rejection but require a second surgical site. Allografts eliminate the need for a second site but carry a small risk of disease transmission. The optimal graft choice depends on individual patient factors, surgeon preference, and the specific reconstruction technique used.
Rehabilitation focuses on restoring range of motion, strength, and proprioception. Initial exercises include pendulum exercises and passive range of motion. As pain subsides, active assisted and active range of motion exercises are introduced. Strengthening exercises progress from isometric contractions to resistance band exercises and eventually to weight training. Proprioceptive exercises help restore shoulder stability and coordination.
While surgery is typically recommended, non-surgical management may involve immobilization in a sling, pain medication, and physical therapy. However, these treatments generally provide limited long-term relief and are less effective at restoring shoulder function compared to surgical reconstruction. Non-surgical options are best suited for patients with minimal symptoms and low functional demands.
In summary, type 3 acromioclavicular joint injuries represent a significant orthopedic challenge requiring careful diagnosis and treatment. Understanding the anatomy, biomechanics, and classification of these injuries is crucial for making informed decisions. Surgical reconstruction, coupled with a comprehensive rehabilitation program, remains the gold standard for restoring shoulder stability and function in most cases.
Looking ahead, advancements in surgical techniques, biomaterials, and rehabilitation protocols hold promise for further improving outcomes. Continued research and innovation are essential to optimize treatment strategies and enhance the quality of life for individuals affected by type 3 AC joint injuries. For more information and consultation, visit our website: www.rays-casting.com.