- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
The shoulder synovial joint, a complex and crucial component of the human musculoskeletal system, enables a remarkable range of motion essential for daily activities. Understanding its anatomy, biomechanics, and potential pathologies is paramount for healthcare professionals, athletes, and anyone seeking to maintain optimal shoulder function. The global impact of shoulder injuries and conditions is significant, affecting millions and contributing to substantial healthcare costs. This exploration delves into the intricacies of the shoulder synovial joint, its applications, and future directions.
Globally, shoulder pain ranks among the most common musculoskeletal complaints, impacting productivity and quality of life. According to the World Health Organization, musculoskeletal conditions are a leading cause of disability worldwide. The aging population, coupled with increasing participation in sports and physically demanding occupations, contributes to a rising incidence of shoulder disorders. Addressing these issues necessitates a deep understanding of the shoulder synovial joint and advancements in diagnostic and therapeutic interventions. This knowledge is not confined to clinical settings; it influences athletic training, ergonomic design, and preventative healthcare strategies.
The shoulder synovial joint, in its simplest definition, is the articulation between the humerus (upper arm bone) and the scapula (shoulder blade). This joint is classified as a ball-and-socket joint, allowing for multiplanar movement. It's a synovial joint, meaning it contains a fluid-filled cavity (the synovial cavity) that lubricates the joint surfaces and reduces friction. This complex structure is critical for a wide array of movements, from reaching overhead to rotating the arm, and its functionality directly impacts our ability to perform countless everyday tasks.

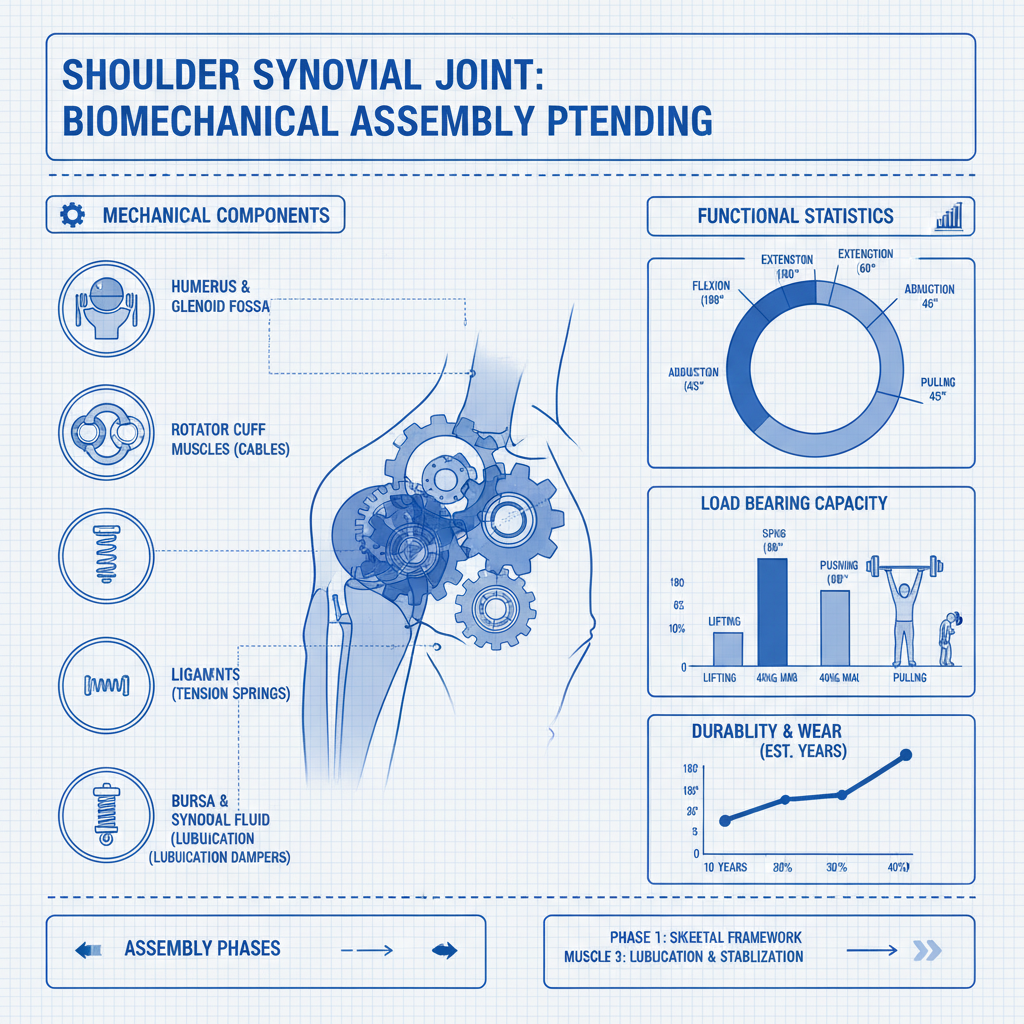
The shoulder synovial joint isn’t a single joint, but a complex of several interacting articulations. These include the glenohumeral joint (the primary ball-and-socket joint), the acromioclavicular (AC) joint, and the sternoclavicular (SC) joint. Each component contributes uniquely to the overall range of motion and stability of the shoulder. The coordinated function of these joints is critical for efficient and pain-free movement.
Understanding the shoulder synovial joint's intricate structure is fundamental to diagnosing and treating various shoulder conditions. Its susceptibility to injury stems from its inherent instability, which allows for a wide range of motion but also makes it vulnerable to dislocations, impingement, and rotator cuff tears. Therefore, a holistic approach to shoulder health requires a detailed understanding of its anatomy and biomechanics.
The glenohumeral joint is the main player, with the head of the humerus articulating with the glenoid fossa of the scapula. This 'ball-and-socket' arrangement offers exceptional mobility but limited inherent stability. The labrum, a fibrocartilaginous rim surrounding the glenoid fossa, deepens the socket and enhances stability. Crucially, the rotator cuff muscles – supraspinatus, infraspinatus, teres minor, and subscapularis – envelop the joint, providing dynamic stability and controlling movement.
Beyond the bony structures and muscles, several ligaments contribute to shoulder stability. The glenohumeral ligaments, superior, middle, and inferior, reinforce the joint capsule. The coracohumeral ligament further limits external rotation. The joint capsule itself is a vital element, enclosing the synovial fluid which lubricates the joint surfaces and reduces friction during movement.
The acromioclavicular (AC) joint, where the acromion of the scapula meets the clavicle, provides a connection between the upper limb and the axial skeleton. This joint is stabilized by the AC ligaments, which are vulnerable to injury, commonly leading to AC joint sprains or dislocations. The sternoclavicular (SC) joint, connecting the clavicle to the sternum, is the only bony connection between the upper limb and the torso and plays a role in transmitting forces.
The shoulder synovial joint’s biomechanics are remarkably complex. Its ability to perform numerous movements – flexion, extension, abduction, adduction, internal rotation, and external rotation – stems from the coordinated action of multiple muscle groups and the unique geometry of the joint surfaces. The scapula plays a critical role, providing a stable base for the humeral head and contributing significantly to overall shoulder motion.
Scapulohumeral rhythm describes the coordinated movement between the scapula and humerus during arm elevation. For every two degrees of humeral elevation, one degree occurs at the glenohumeral joint, and one degree occurs through scapular upward rotation. Disruptions in this rhythm can lead to impingement syndromes and other shoulder dysfunctions. Understanding this rhythm is crucial for effective rehabilitation programs.
Joint congruency, the degree of fit between the humeral head and the glenoid fossa, is relatively low in the shoulder. This inherent instability allows for a large range of motion, but also necessitates robust dynamic stabilization provided by the rotator cuff muscles and surrounding ligaments. Maintaining optimal muscle strength and coordination is paramount for preventing injury and preserving shoulder function.
Numerous conditions can affect the shoulder synovial joint, ranging from acute injuries to chronic degenerative changes. Rotator cuff tears, often resulting from repetitive overhead activities or traumatic injury, are a common source of shoulder pain and disability. Impingement syndrome, where tendons become compressed within the shoulder joint, is another frequent complaint.
Shoulder instability, characterized by a feeling of looseness or dislocation, can stem from ligament laxity, labral tears, or recurrent subluxations. Adhesive capsulitis, or “frozen shoulder,” involves inflammation and stiffness of the joint capsule, severely limiting range of motion. Osteoarthritis, a degenerative joint disease, can also affect the shoulder, leading to pain, stiffness, and decreased function.
Conservative management for shoulder synovial joint conditions often involves a multifaceted approach, including physical therapy, pain medication, and activity modification. Physical therapy focuses on restoring range of motion, strengthening surrounding muscles (particularly the rotator cuff), and improving scapular mechanics.
Pain management strategies may include over-the-counter analgesics, nonsteroidal anti-inflammatory drugs (NSAIDs), or, in some cases, corticosteroid injections. Activity modification involves avoiding activities that exacerbate symptoms and adopting proper biomechanics during daily tasks. Early intervention and adherence to a rehabilitation program are crucial for optimal outcomes.
When conservative management fails to provide adequate relief, surgical intervention may be considered. Arthroscopic surgery, a minimally invasive technique, is frequently used to address rotator cuff tears, labral tears, and impingement syndromes. Open surgery may be necessary for more complex cases, such as severe rotator cuff tears or shoulder instability requiring ligament reconstruction.
Shoulder replacement surgery, or arthroplasty, is an option for patients with advanced osteoarthritis or irreparable rotator cuff tears. Various types of shoulder replacements are available, including total shoulder replacement and reverse total shoulder replacement, tailored to individual patient needs. Postoperative rehabilitation is crucial for restoring function and achieving optimal outcomes.
Surgical techniques are continuously evolving, with advancements in arthroscopic procedures and implant designs aiming to improve patient outcomes and minimize recovery times.
The field of shoulder synovial joint care is witnessing exciting innovations. Biologic therapies, such as platelet-rich plasma (PRP) and stem cell injections, are being investigated for their potential to promote tissue healing and reduce pain. Advanced imaging techniques, such as dynamic MRI, are improving diagnostic accuracy and guiding treatment decisions.
Robotic-assisted surgery is emerging as a promising tool for enhancing surgical precision and minimizing invasiveness. Virtual reality and augmented reality technologies are being used to develop innovative rehabilitation programs and improve patient engagement. Research into tissue engineering and regenerative medicine holds the potential for future breakthroughs in shoulder joint repair.
| Diagnosis | Treatment Modality | Rehabilitation Focus | Expected Outcome |
|---|---|---|---|
| Rotator Cuff Tear | Arthroscopic Repair/Tendon Transfer | Range of Motion, Rotator Cuff Strengthening | Pain Reduction, Improved Function (6-12 months) |
| Impingement Syndrome | Physical Therapy, Subacromial Decompression | Posture Correction, Scapular Stabilization | Pain Relief, Improved Overhead Motion (2-6 months) |
| Shoulder Instability | Arthroscopic Stabilization (Bankart Repair) | Rotator Cuff & Scapular Muscle Strengthening | Restored Stability, Return to Activity (6-9 months) |
| Adhesive Capsulitis | Physical Therapy, Hydrodilatation | Aggressive Range of Motion Exercises | Improved Range of Motion (6-18 months) |
| Osteoarthritis | Pain Management, Joint Replacement | Muscle Strengthening, Low-Impact Exercise | Pain Relief, Improved Function (Varies) |
| Labral Tear | Arthroscopic Labral Repair | Rotator Cuff Strengthening, Proprioceptive Training | Pain Reduction, Improved Stability (4-6 Months) |
Recovery from rotator cuff repair varies depending on the size and complexity of the tear, as well as individual factors. Generally, a full recovery can take 6-12 months. The initial phase (0-6 weeks) focuses on pain control and protecting the repair. Gradual rehabilitation then progresses through range of motion, strengthening, and functional activities. Adherence to the physical therapy protocol is critical for optimal results.
Preventing shoulder impingement involves addressing biomechanical factors and strengthening the muscles that control shoulder movement. Maintaining good posture, avoiding repetitive overhead activities, and performing regular exercises to strengthen the rotator cuff and scapular stabilizers are key. Proper warm-up and cool-down routines are also important. Consider ergonomic adjustments in the workplace to minimize strain on the shoulder.
Signs of a labral tear can include a deep, aching pain in the shoulder, a sensation of clicking or popping, and a feeling of instability. Pain may be aggravated by overhead activities or reaching across the body. A specific maneuver, known as the O'Brien test, can help your physician assess for a labral tear. Imaging studies, such as MRI, can also aid in diagnosis.
Surgery is not always necessary for adhesive capsulitis. The vast majority of cases respond well to conservative management, including physical therapy, pain medication, and corticosteroid injections. Hydrodilatation, a procedure that involves injecting fluid into the joint capsule to stretch it, can also be helpful. Surgery is typically reserved for cases that fail to improve with conservative treatment after 6-12 months.
The scapula plays a vital role in shoulder function, acting as the foundation for arm movement. Proper scapular positioning and movement (scapulohumeral rhythm) are essential for optimal shoulder mechanics. Weakness or dysfunction of the muscles that control the scapula can lead to shoulder pain and dysfunction. Strengthening these muscles is a key component of shoulder rehabilitation.
Returning to sports after shoulder surgery requires a careful and individualized rehabilitation program. The timeline for return to play varies depending on the type of surgery, the individual's healing progress, and the demands of the sport. A gradual progression of activities is essential, starting with range of motion and strengthening exercises and progressing to sport-specific drills. Clearance from your surgeon and physical therapist is crucial before returning to competitive play.
The shoulder synovial joint is a remarkably complex and vital structure, enabling a wide range of motion essential for daily life. A thorough understanding of its anatomy, biomechanics, and common pathologies is crucial for effective diagnosis, treatment, and prevention of shoulder disorders. From conservative management to cutting-edge surgical techniques, a diverse array of options exists to address shoulder pain and restore function.
Looking ahead, continued research and innovation promise to further refine our understanding of the shoulder synovial joint and lead to even more effective treatments. Emphasis on preventative strategies, such as proper exercise technique and ergonomic adjustments, will be paramount in reducing the incidence of shoulder injuries. For more information and resources, please visit our website: rays-casting.com.