- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
Type 3 clavicle fracture, a complete displacement of the clavicle with significant comminution, presents a complex orthopedic challenge. Understanding its biomechanics, treatment options, and potential complications is crucial for optimal patient outcomes. These fractures, often resulting from high-energy trauma, require meticulous management to restore shoulder function and minimize long-term disability. Proper diagnosis and tailored treatment plans are essential for individuals impacted by this injury.
The global incidence of clavicle fractures is approximately 5-10% of all upper extremity fractures, with type 3 fractures representing a smaller but significant subset. These injuries are prevalent in traffic accidents, falls, and sports-related impacts, impacting a broad demographic. Increased urbanization, motor vehicle density, and participation in high-risk recreational activities contribute to the sustained incidence of these fractures worldwide.
Effective management of type 3 clavicle fracture is paramount for reducing morbidity and improving quality of life. The availability of advanced surgical techniques and rehabilitation protocols has dramatically enhanced outcomes. However, disparities in access to quality healthcare in many regions necessitate a focus on affordable and effective treatment strategies. Understanding the nuances of this fracture type allows healthcare professionals to provide specialized care.
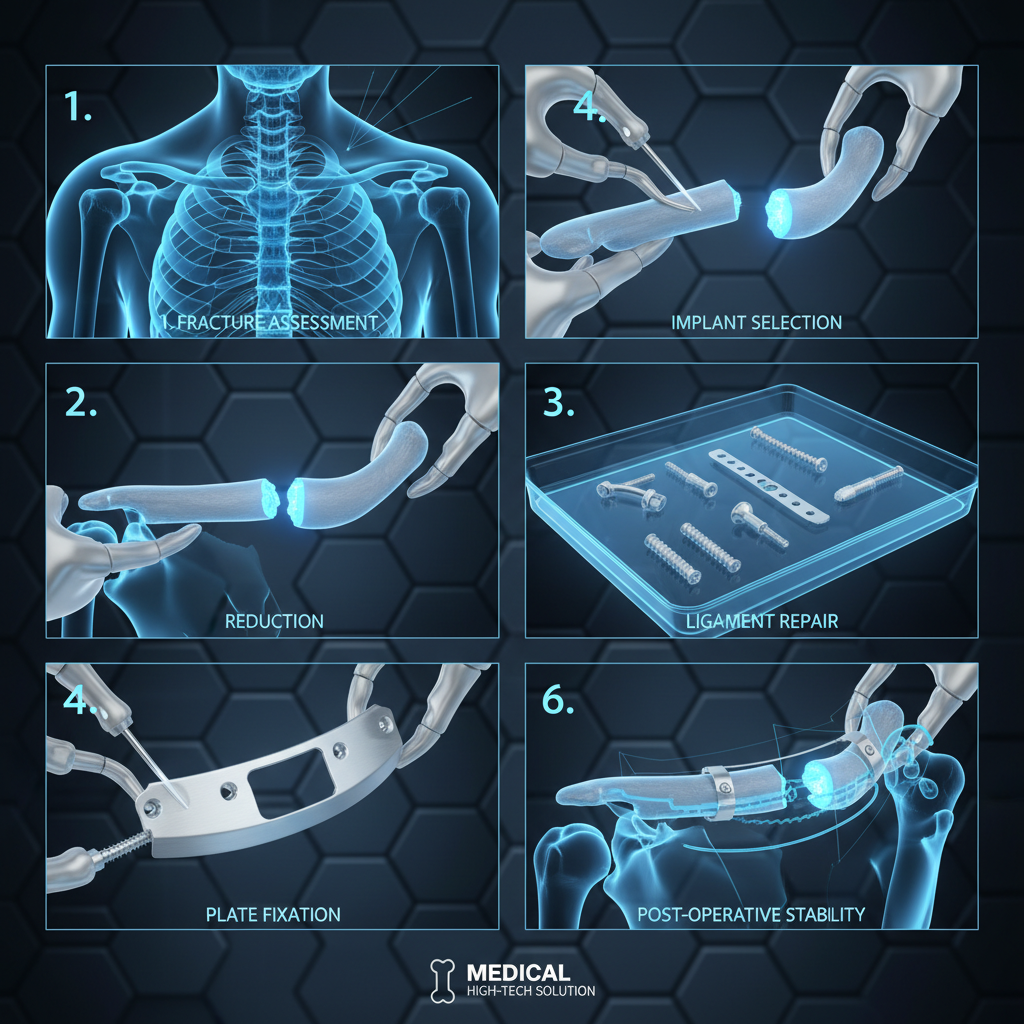
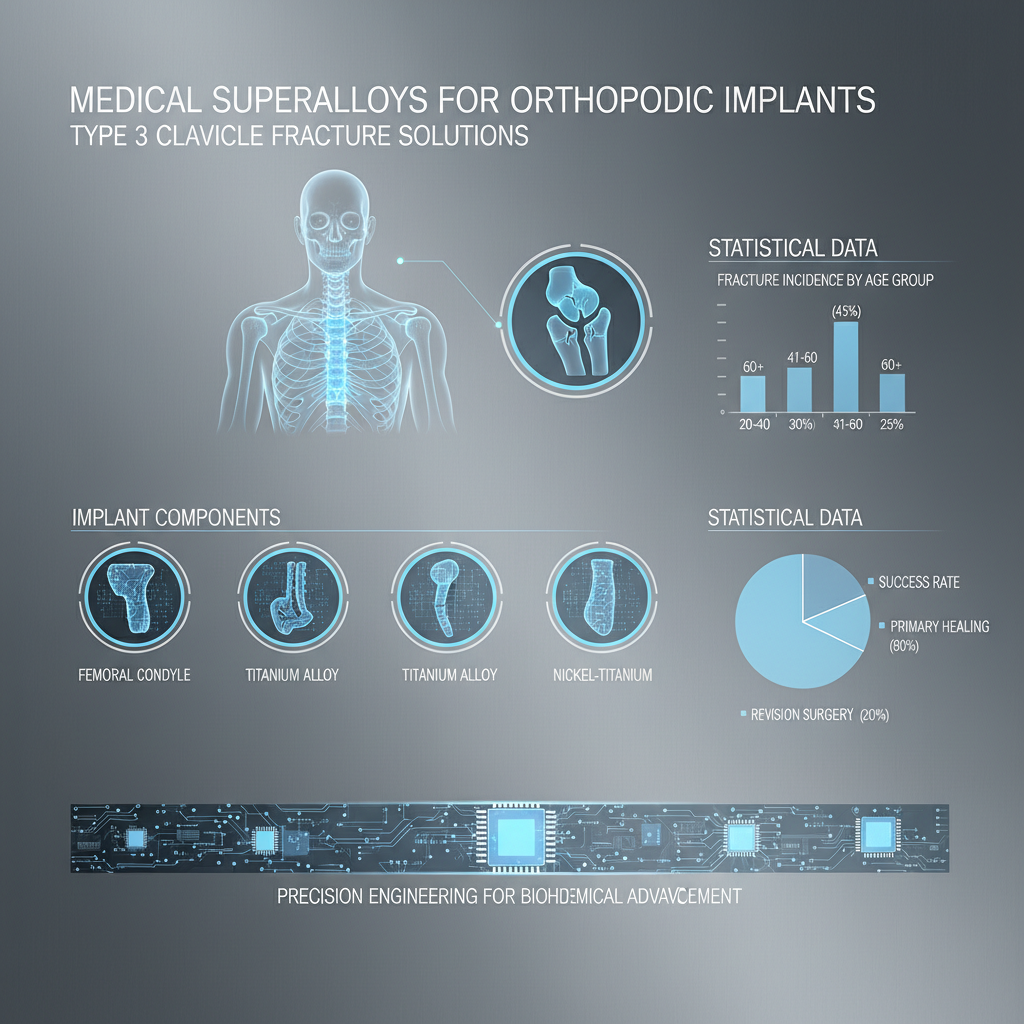
A type 3 clavicle fracture, as defined by the Neer classification, is a complete fracture of the clavicle shaft with significant displacement of the bone fragments. This fracture often involves multiple fracture fragments (comminution), which can complicate the healing process. This contrasts with type 1 and 2 fractures, which are less severe.
The severity of a type 3 clavicle fracture stems from the instability inherent in the fracture pattern. The weight of the upper extremity and the pull of the surrounding muscles tend to pull the fractured segments apart, hindering natural healing. Therefore, surgical intervention is frequently required to achieve stable fixation and restore proper alignment.
The clavicle, acting as a strut connecting the upper extremity to the axial skeleton, is susceptible to fractures due to its exposed position and relatively thin cortical bone. Type 3 clavicle fractures typically occur when a substantial force is applied to the midshaft of the bone. The mechanism of injury often involves a direct blow or a fall onto the shoulder.
The forces involved in a type 3 clavicle fracture not only break the bone but also disrupt the surrounding soft tissues, including the periosteum, muscles, and ligaments. This disruption contributes to the instability of the fracture and influences the healing process. Understanding these biomechanical principles is essential for selecting the most appropriate treatment strategy.
The tension and compression forces acting on the clavicle during injury are crucial in determining the fracture pattern. Comminution, a hallmark of type 3 fractures, is often a result of bending forces exceeding the bone's tensile strength. This results in multiple bone fragments requiring stabilization.
Accurate diagnosis of a type 3 clavicle fracture begins with a thorough clinical examination. Patients typically present with pain, swelling, and deformity around the clavicle. Neurovascular assessment is essential to rule out any associated injuries to the nerves and blood vessels in the area.
Radiographic imaging, specifically anteroposterior (AP) and cephalic tilt views of the clavicle, is the cornerstone of diagnosis. These X-rays clearly visualize the fracture pattern, degree of displacement, and presence of comminution. In some cases, a computed tomography (CT) scan may be necessary to provide a more detailed assessment of the fracture fragments and surrounding structures.
The goal of diagnostic imaging is not only to confirm the presence of a fracture but also to classify it accurately according to the Neer classification. This classification system guides treatment decisions and helps predict the potential for complications. Careful interpretation of the radiographic findings is paramount.
Treatment for a type 3 clavicle fracture is often surgical, although non-operative management may be considered in carefully selected cases. Surgical fixation typically involves open reduction and internal fixation (ORIF) with a plate and screws. This provides stability to the fracture site and allows for early mobilization.
Non-operative treatment, such as immobilization in a sling, is generally reserved for patients with minimal displacement, acceptable alignment, and no neurovascular compromise. However, non-operative treatment carries a higher risk of nonunion (failure of the fracture to heal) and malunion (healing in a suboptimal position).
Surgical techniques for type 3 clavicle fracture vary globally, influenced by factors such as surgeon preference, resource availability, and healthcare systems. In developed countries, plate and screw fixation is the most common approach, offering excellent stability and functional outcomes.
In resource-limited settings, alternative fixation methods, such as intramedullary nailing or elastic nailing, may be employed due to their lower cost and technical demands. However, these techniques may be associated with a higher risk of complications and slower healing times. Standardization of surgical protocols and training are crucial for optimizing care worldwide.
Postoperative rehabilitation is a critical component of recovery following type 3 clavicle fracture repair. A structured rehabilitation program, guided by a physical therapist, aims to restore range of motion, strength, and function of the shoulder.
Potential complications of type 3 clavicle fracture include nonunion, malunion, infection, nerve injury, and hardware failure. Close monitoring and prompt intervention are essential to address these complications and optimize long-term outcomes. Patients should be educated about the signs and symptoms of complications and instructed to seek medical attention if they arise.
Long-term follow-up is important to assess for persistent pain, stiffness, or functional limitations. Individuals who have sustained a type 3 clavicle fracture may require ongoing physical therapy or pain management to maintain optimal shoulder function.
Ongoing research is focused on developing new and improved treatment strategies for type 3 clavicle fractures. Biologic augmentation techniques, such as platelet-rich plasma (PRP) or bone marrow aspirate concentrate (BMAC), are being investigated to enhance fracture healing.
The development of novel fixation devices, including biodegradable implants and patient-specific plates, holds promise for minimizing complications and improving functional outcomes. Advanced imaging modalities, such as 3D printing and virtual surgical planning, may also play a role in optimizing treatment planning.
Furthermore, advancements in regenerative medicine offer the potential to stimulate bone healing and restore tissue regeneration in cases of nonunion or malunion. Continuous innovation and collaboration are essential to advance the field of clavicle fracture care.
| Fracture Severity | Patient Age & Health | Treatment Approach | Rehabilitation Compliance |
|---|---|---|---|
| High comminution, displacement | Older age, comorbidities | ORIF with plate and screws | Excellent adherence to protocol |
| Moderate comminution, minimal displacement | Younger age, good health | Non-operative management | Good adherence, but slower progress |
| Significant displacement, unstable fracture | Smoking history, diabetes | ORIF with bone grafting | Moderate adherence, potential delays |
| Minor comminution, stable fracture | Active lifestyle, high functional demands | Minimally invasive ORIF | High motivation, rapid recovery |
| Complex fracture pattern | Osteoporosis, poor bone quality | Augmented fixation with biologics | Cautious progression, pain management |
| Delayed presentation, chronic fracture | Multiple medical conditions | Reconstructive surgery | Realistic expectations, long-term management |
The recovery timeline varies, but generally, patients can expect to wear a sling for 6-8 weeks post-surgery. Gradual range-of-motion exercises begin around 6 weeks, progressing to strengthening exercises over the next several months. Full functional recovery, including return to sports, may take 6-12 months. Regular follow-up with an orthopedic surgeon and physical therapist is crucial.
Non-operative management carries a higher risk of nonunion (failure of the fracture to heal), malunion (healing in a suboptimal position), and persistent pain. It can also lead to limited shoulder range of motion and reduced strength. Careful patient selection and close monitoring are essential when considering non-operative treatment.
Smoking significantly impairs fracture healing by reducing blood flow to the fracture site and interfering with bone formation. Smokers have a higher risk of nonunion, delayed union, and infection. Smoking cessation is strongly recommended before and after surgery to optimize healing outcomes.
Physical therapy is integral to restoring shoulder function after a type 3 clavicle fracture. A tailored program addresses pain management, range of motion, strengthening, and proprioception. Therapists guide patients through progressive exercises to regain full use of their arm and shoulder.
Signs of delayed or nonunion include persistent pain, inability to bear weight on the affected arm, and continued visible displacement of the fracture fragments on X-rays. Prompt evaluation by an orthopedic surgeon is necessary if any of these signs are present.
While not inevitable, a type 3 clavicle fracture can increase the risk of developing arthritis in the acromioclavicular (AC) joint over time. This is especially true if the fracture involved the AC joint or if the fracture healing was not optimal. Maintaining proper shoulder mechanics and avoiding excessive stress on the joint can help minimize this risk.
In summary, type 3 clavicle fractures are complex injuries requiring careful diagnosis and tailored treatment. Understanding the fracture mechanics, available treatment modalities, and potential complications is crucial for achieving optimal patient outcomes. Surgical fixation remains the gold standard for unstable fractures, while diligent rehabilitation is essential for restoring shoulder function.
Continued research into new fixation techniques, biologic augmentation, and regenerative medicine promises to further improve the care of patients with type 3 clavicle fractures. For more information and access to expert orthopedic care, please visit our website at www.rays-casting.com.
