- Tel: +8613911709825 /
- Email: ry@rays-casting.com /
The humerus ball and socket joint, a cornerstone of upper limb functionality, is a globally relevant topic due to its implications for healthcare, rehabilitation, and athletic performance. Understanding its biomechanics, potential pathologies, and treatment options is critical for medical professionals worldwide. This joint's robust design and wide range of motion contribute significantly to human dexterity and quality of life, impacting everything from daily tasks to specialized professions.
The prevalence of shoulder-related injuries, including those impacting the humerus ball and socket, is steadily increasing, driven by factors like aging populations, repetitive strain from modern work, and increased participation in sports. This presents a substantial global healthcare challenge, necessitating advancements in diagnostics, preventative measures, and restorative therapies. Effective management of conditions affecting this joint leads to reduced disability and improved patient outcomes.
The study and improvement of the humerus ball and socket joint extends beyond clinical medicine. Engineering applications, such as the development of prosthetic limbs and robotic assistance devices, directly benefit from a detailed understanding of its structure and function. Furthermore, athletic training and performance optimization rely heavily on maximizing the joint’s capabilities while minimizing the risk of injury.
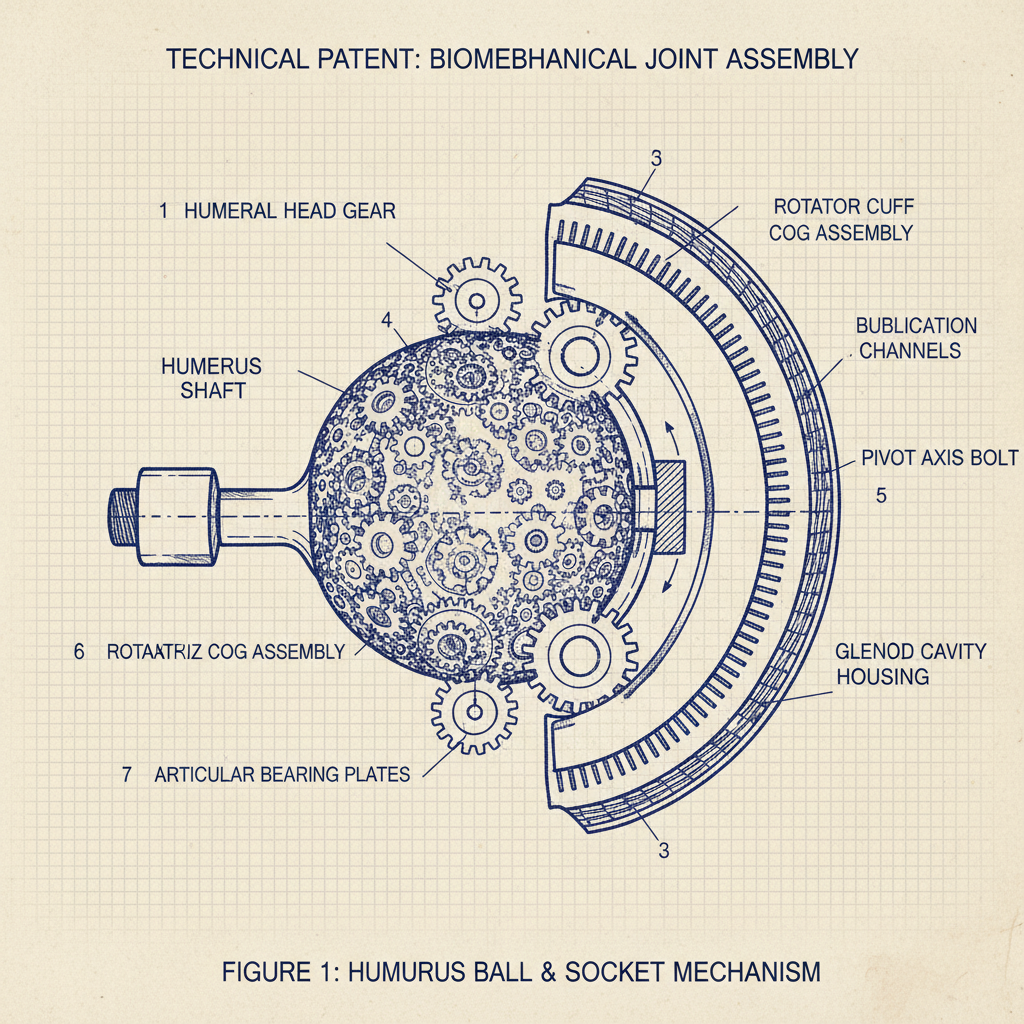

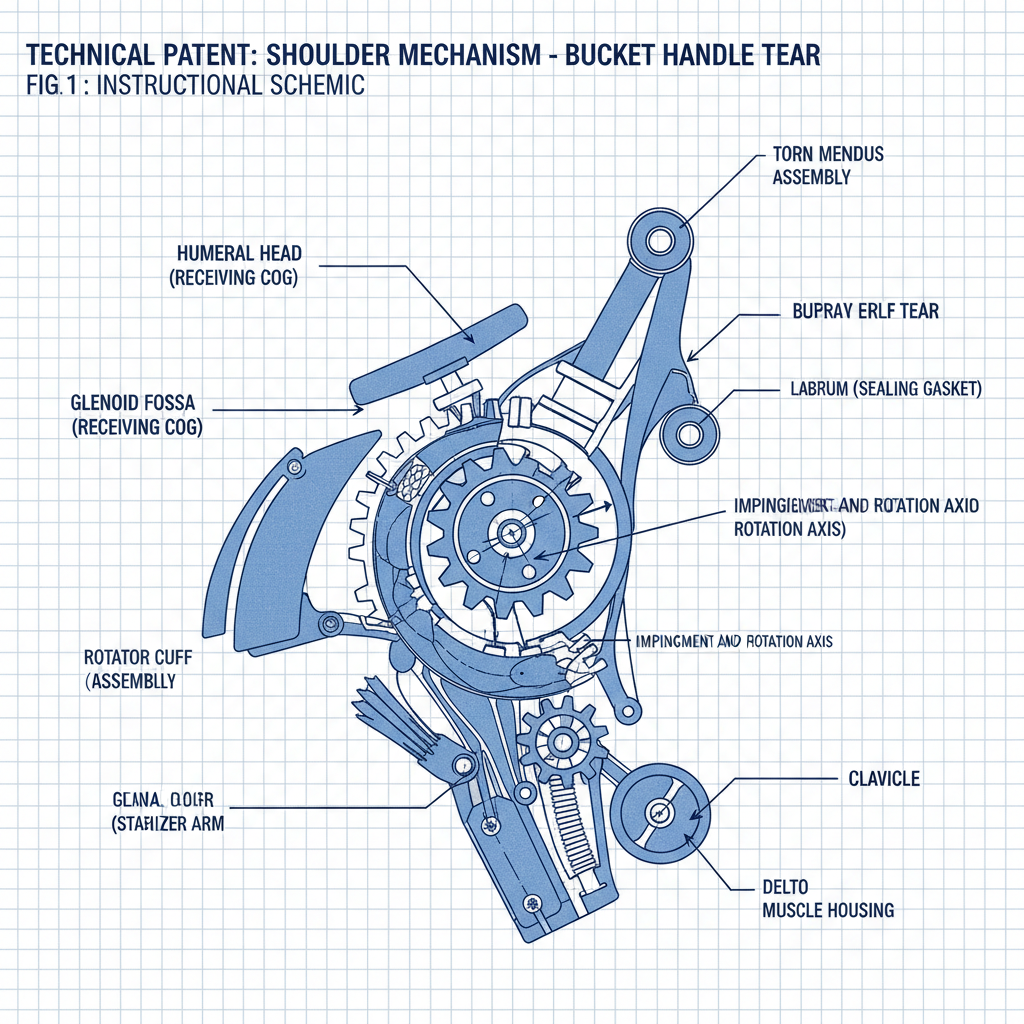
The humerus ball and socket joint, also known as the glenohumeral joint, is a synovial joint formed by the articulation of the head of the humerus (the ‘ball’) with the glenoid fossa of the scapula (the ‘socket’). This articulation allows for a vast range of motion in the shoulder, including flexion, extension, abduction, adduction, internal and external rotation, and circumduction.
Several key structures contribute to the stability of the humerus ball and socket. These include the glenoid labrum, a fibrocartilaginous rim that deepens the glenoid fossa; the rotator cuff muscles (supraspinatus, infraspinatus, teres minor, and subscapularis), which provide dynamic stabilization and control movement; and the glenohumeral ligaments, which offer static support. Understanding these anatomical components is essential for diagnosing and treating related conditions.
The inherent instability of the humerus ball and socket is a defining characteristic, contributing to its wide range of motion. The relatively small size of the glenoid fossa compared to the humeral head means that the joint relies heavily on soft tissue structures for stability. This makes it susceptible to dislocation and subluxation, particularly with forceful movements or trauma. The biomechanics of scapular motion also play a crucial role; proper scapulothoracic rhythm is essential for optimal shoulder function.
The rotator cuff muscles exert complex forces on the humeral head, compressing it against the glenoid fossa and maintaining joint stability. The interplay between these muscles and the surrounding ligaments dictates the shoulder's ability to resist translational forces and rotational stresses. Age-related degeneration of these tissues can significantly impair these biomechanical properties, increasing the risk of injury and functional decline.
The humerus ball and socket joint’s kinematic chain extends beyond just the shoulder, integrating with the cervical spine, thoracic cage, and scapula. Efficient movement and stability require coordinated action of all these components. Analyzing movement patterns and identifying biomechanical inefficiencies is crucial for effective rehabilitation and prevention programs.
A wide range of pathologies can affect the humerus ball and socket, from acute traumatic injuries to chronic degenerative conditions. Rotator cuff tears are among the most common, often resulting from overuse, age-related degeneration, or acute trauma. These tears can lead to pain, weakness, and limited range of motion.
Impingement syndrome, where tendons or bursae are compressed within the shoulder joint, is another frequent complaint. This can result from anatomical abnormalities, poor posture, or repetitive overhead activities. Adhesive capsulitis, or “frozen shoulder,” is characterized by stiffness and pain in the shoulder, limiting all ranges of motion. Glenohumeral osteoarthritis, a degenerative joint disease, can develop over time due to wear and tear, leading to cartilage breakdown and bone spurs.
Instability, encompassing dislocation and subluxation, often occurs following traumatic events, although chronic instability can develop due to repetitive microtrauma. Labral tears, affecting the glenoid labrum, are also common, frequently presenting as clicking, popping, or a sensation of instability in the shoulder. These pathologies often overlap and require a comprehensive diagnostic approach.
Accurate diagnosis of humerus ball and socket pathologies requires a thorough clinical examination, including a detailed history of the patient's symptoms, activity level, and any prior injuries. Range of motion assessment, strength testing, and specific provocative maneuvers are crucial components of the physical examination.
Treatment for humerus ball and socket injuries varies significantly depending on the specific diagnosis, severity of symptoms, and individual patient factors. Conservative management, including rest, ice, compression, and elevation (RICE), is often the first line of defense for mild to moderate injuries. Physical therapy plays a vital role in restoring range of motion, strengthening surrounding muscles, and improving functional capacity.
For more severe injuries, such as complete rotator cuff tears or significant instability, surgical intervention may be necessary. Arthroscopic surgery, a minimally invasive technique, is frequently used to repair torn tissues, stabilize the joint, and address impingement syndrome. Open surgical procedures may be required for complex reconstructions or revisions.
Post-operative rehabilitation following humerus ball and socket surgery is crucial for a successful outcome. A structured program, guided by a physical therapist, progresses through phases focusing on pain control, range of motion recovery, strengthening, and functional reintegration. Compliance with the rehabilitation protocol is essential for optimal healing and return to activity.
Preventive strategies are equally important for minimizing the risk of future injuries. These include proper warm-up and cool-down routines, strengthening exercises for the rotator cuff and scapular stabilizers, and maintaining good posture. Avoiding overuse, modifying activities that exacerbate symptoms, and addressing biomechanical imbalances can also help protect the humerus ball and socket.
Education on proper lifting techniques and activity modification is also key.
Ongoing research continues to refine our understanding of the humerus ball and socket joint and develop innovative treatment approaches. Biomechanical modeling and advanced imaging techniques are being used to study joint kinematics and identify risk factors for injury. Regenerative medicine strategies, such as platelet-rich plasma (PRP) injections and stem cell therapy, are showing promise in promoting tissue healing and reducing pain.
The development of more sophisticated prosthetic shoulder joints and robotic assistance devices is also advancing rapidly. These technologies aim to restore function and improve quality of life for individuals with severe shoulder pathology. Furthermore, personalized rehabilitation programs, tailored to the individual patient's needs and genetic predisposition, are becoming increasingly prevalent.
Artificial intelligence (AI) is being integrated into diagnostic tools and rehabilitation programs, offering the potential for more accurate diagnoses and personalized treatment plans.
| Research Area | Potential Impact | Current Challenges | Estimated Timeline |
|---|---|---|---|
| Regenerative Medicine (PRP, Stem Cells) | Enhanced tissue healing, reduced pain, potentially avoiding surgery | Optimizing cell delivery, long-term efficacy, cost-effectiveness | 5-10 years |
| AI-Driven Diagnostics | Earlier and more accurate diagnoses, personalized treatment recommendations | Data availability, algorithm validation, ethical considerations | 3-7 years |
| Biomechanical Modeling | Improved understanding of joint kinematics, risk factor identification | Model complexity, accurate representation of soft tissues | Ongoing |
| Advanced Prosthetic Joints | Restoration of function, improved range of motion, reduced pain | Biocompatibility, durability, integration with the nervous system | 7-15 years |
| Personalized Rehabilitation | Optimized recovery, faster return to activity, reduced risk of re-injury | Data collection, algorithm development, patient compliance | 3-5 years |
| Robotic Assistance Devices | Enhanced surgical precision, improved rehabilitation outcomes | Cost, complexity, integration with surgical workflows | 5-10 years |
Early signs of a rotator cuff tear often include a dull aching pain deep in the shoulder, particularly at night. Pain may worsen with overhead activities or reaching behind the back. You might experience difficulty lifting or rotating your arm, and may notice weakness. Ignoring these symptoms can lead to more significant tears and functional limitations. Early intervention, including physical therapy, can often help manage symptoms and prevent progression.
Recovery from rotator cuff surgery varies depending on the size and complexity of the tear, as well as individual factors. Generally, the initial phase (0-6 weeks) focuses on pain control and range of motion. Strengthening exercises begin around 6-12 weeks, with a gradual return to functional activities over the next several months. Full recovery and return to sports can take 6-12 months or longer. Adhering to the rehabilitation protocol is crucial for optimal outcomes.
Adhesive capsulitis can sometimes resolve on its own over a period of 1-3 years, but this is often accompanied by significant pain and functional limitations. Physical therapy is highly effective in accelerating the recovery process and improving range of motion. In some cases, corticosteroid injections or manipulation under anesthesia may be necessary to break up adhesions and restore joint mobility. Early intervention can significantly improve outcomes.
Several preventative measures can help protect your shoulder joint. Regularly perform rotator cuff and scapular strengthening exercises. Maintain good posture, especially when sitting and lifting. Warm up properly before physical activity, and avoid overuse or repetitive motions. Use proper lifting techniques, and address any biomechanical imbalances. Listen to your body and seek medical attention if you experience persistent shoulder pain.
Scapular stability is fundamental to proper shoulder function. The scapula provides a stable base for the humerus to move, and proper scapulothoracic rhythm is crucial for efficient movement. Weakness or dysfunction of the scapular stabilizers (such as serratus anterior and lower trapezius) can lead to altered biomechanics, impingement, and increased risk of injury. Targeted exercises to strengthen these muscles are essential for maintaining shoulder health.
Yes, several non-surgical options can help manage shoulder osteoarthritis. These include physical therapy to maintain range of motion and strengthen surrounding muscles, pain medication (over-the-counter or prescription), corticosteroid injections, and hyaluronic acid injections. Lifestyle modifications, such as weight loss and activity modification, can also help reduce stress on the joint. While these options may not cure osteoarthritis, they can effectively manage symptoms and improve quality of life.
In conclusion, the humerus ball and socket joint is a remarkably complex and vital structure, central to upper limb function and impacting countless aspects of daily life. Understanding its anatomy, biomechanics, and common pathologies is critical for healthcare professionals, athletes, and individuals seeking to maintain optimal shoulder health. Advancements in diagnostics, treatment, and rehabilitation continue to improve outcomes and enhance quality of life for those affected by shoulder conditions.
Looking ahead, continued research into regenerative medicine, AI-driven diagnostics, and personalized rehabilitation promises to revolutionize the field. By embracing these innovations and prioritizing preventative measures, we can strive to minimize the burden of shoulder pain and injury, empowering individuals to maintain an active and fulfilling lifestyle. For more in-depth information and expert guidance, visit our website: rays-casting.com